Abstract
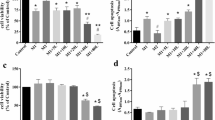
Macrophages (Mϕs) play an important role in the inflammatory response during injury by participating in the removal of injurious stimuli, such as bacteria, and promoting tissue healing to restore homeostasis. Mϕs can acquire distinct functional phenotypes along a spectrum between two opposite stages (M1/M2) during activation. In the present study, we induced a stress response in Mϕs via heat shock (HS) and found that it incurred an increase in phagocytosis (1.6-fold, P < 0.05) and bacterial killing (2.8-fold, P < 0.01). Upon heat stress activation, Mϕs respond to group B Streptococcus (GBS) infection with lower levels of pro-inflammatory cytokines, TNF-α (2.25-fold, P < 0.01), IL-6 (7-fold, P < 0.001), and inducible nitric oxide synthase (iNOS) (2.22-fold, P < 0.05), but higher levels of the anti-inflammatory cytokine IL-10 (3.9-fold, P < 0.01). Stressed Mϕs exposed to GBS display rapid phagosome maturation, increased extracellular trap (ET) formation and elevated cathelicidin antimicrobial peptide expression (2.5-fold, P < 0.001). These findings are consistent with a heretofore uncharacterized Mϕ activation state formed in response to stress, associated with secretion of large quantities of anti-inflammatory mediators and redirection of antimicrobial mechanisms to NADPH-oxidase-independent pathways. This “friendly activation” of Mϕs is characterized by increased bactericidal activity and more rapid and controlled resolution of the inflammatory response.
Key Messages
-
Macrophages form a dual pro-bactericidal and anti-inflammatory state.
-
Stress in the setting of infection triggers friendly activation in macrophages.
-
Heat shock plus infection increases macrophage bactericidal activity.
-
Heat shock plus infection increases macrophage extracellular trap formation.
-
Heat shock plus infection increases macrophage production of cathelicidin and IL-10.






Similar content being viewed by others
References
Liu G, Yang H (2013) Modulation of macrophage activation and programming in immunity. J Cell Physiol 228:502–512
Busse W, Corren J, Lanier BQ, McAlary M, Fowler-Taylor A, Cioppa GD, van As A, Gupta N (2001) Omalizumab, anti-IgE recombinant humanized monoclonal antibody, for the treatment of severe allergic asthma. J Allergy Clin Immunol 108:184–190
van Dullemen HM, van Deventer SJ, Hommes DW, Bijl HA, Jansen J, Tytgat GN, Woody J (1995) Treatment of Crohn’s disease with anti-tumor necrosis factor chimeric monoclonal antibody (cA2). Gastroenterology 109:129–135
Cohen SB, Emery P, Greenwald MW, Dougados M, Furie RA, Genovese MC, Keystone EC, Loveless JE, Burmester GR, Cravets MW et al (2006) Rituximab for rheumatoid arthritis refractory to anti-tumor necrosis factor therapy: results of a multicenter, randomized, double-blind, placebo-controlled, phase III trial evaluating primary efficacy and safety at twenty-four weeks. Arthritis Rheum 54:2793–2806
Biswas SK, Mantovani A (2010) Macrophage plasticity and interaction with lymphocyte subsets: cancer as a paradigm. Nat Immunol 11:889–896
Mosser DM, Edwards JP (2008) Exploring the full spectrum of macrophage activation. Nat Rev Immunol 8:958–969
Gordon S (2003) Alternative activation of macrophages. Nat Rev Immunol 3:23–35
Mantovani A, Sica A, Sozzani S, Allavena P, Vecchi A, Locati M (2004) The chemokine system in diverse forms of macrophage activation and polarization. Trends Immunol 25:677–686
Mantovani A, Sozzani S, Locati M, Schioppa T, Saccani A, Allavena P, Sica A (2004) Infiltration of tumours by macrophages and dendritic cells: tumour-associated macrophages as a paradigm for polarized M2 mononuclear phagocytes. Novartis Found Symp 256:137–145, discussion 146–138, 259–169
Li J, Hsu HC, Mountz JD (2012) Managing macrophages in rheumatoid arthritis by reform or removal. Curr Rheumatol Rep 14:445–454
Liu C, Li Y, Yu J, Feng L, Hou S, Liu Y, Guo M, Xie Y, Meng J, Zhang H et al (2013) Targeting the shift from m1 to m2 macrophages in experimental autoimmune encephalomyelitis mice treated with fasudil. PLoS One 8:e54841
Nazari-Jahantigh M, Wei Y, Noels H, Akhtar S, Zhou Z, Koenen RR, Heyll K, Gremse F, Kiessling F, Grommes J et al (2012) MicroRNA-155 promotes atherosclerosis by repressing Bcl6 in macrophages. J Clin Invest 122:4190–4202
Laskin DL, Pendino KJ (1995) Macrophages and inflammatory mediators in tissue injury. Annu Rev Pharmacol Toxicol 35:655–677
Currie AJ, Curtis S, Strunk T, Riley K, Liyanage K, Prescott S, Doherty D, Simmer K, Richmond P, Burgner D (2011) Preterm infants have deficient monocyte and lymphocyte cytokine responses to group B streptococcus. Infect Immun 79:1588–1596
Vega VL, De Maio A (2005) Increase in phagocytosis after geldanamycin treatment or heat shock: role of heat shock proteins. J Immunol 175:5280–5287
Vega VL, Charles W, De Maio A (2010) A new feature of the stress response: increase in endocytosis mediated by Hsp70. Cell Stress Chaperones 15:517–527
Vega VL, Rodriguez-Silva M, Frey T, Gehrmann M, Diaz JC, Steinem C, Multhoff G, Arispe N, De Maio A (2008) Hsp70 translocates into the plasma membrane after stress and is released into the extracellular environment in a membrane-associated form that activates macrophages. J Immunol 180:4299–4307
Green SA, Kelly RB (1990) Endocytic membrane traffic to the Golgi apparatus in a regulated secretory cell line. J Biol Chem 265:21269–21278
Flesch IE, Kaufmann SH (1991) Mechanisms involved in mycobacterial growth inhibition by gamma interferon-activated bone marrow macrophages: role of reactive nitrogen intermediates. Infect Immun 59:3213–3218
Maridonneau-Parini I, Malawista SE, Stubbe H, Russo-Marie F, Polla BS (1993) Heat shock in human neutrophils: superoxide generation is inhibited by a mechanism distinct from heat-denaturation of NADPH oxidase and is protected by heat shock proteins in thermotolerant cells. J Cell Physiol 156:204–211
Souren JE, Van Der Mast C, Van Wijk R (1997) NADPH-oxidase-dependent superoxide production by myocyte-derived H9c2 cells: influence of ischemia, heat shock, cycloheximide and cytochalasin D. J Mol Cell Cardiol 29:2803–2812
Maridonneau-Parini I, Clerc J, Polla BS (1988) Heat shock inhibits NADPH oxidase in human neutrophils. Biochem Biophys Res Commun 154:179–186
Glaser P, Rusniok C, Buchrieser C, Chevalier F, Frangeul L, Msadek T, Zouine M, Couve E, Lalioui L, Poyart C et al (2002) Genome sequence of Streptococcus agalactiae, a pathogen causing invasive neonatal disease. Mol Microbiol 45:1499–1513
Vega VL, De Cabo R, De Maio A (2004) Age and caloric restriction diets are confounding factors that modify the response to lipopolysaccharide by peritoneal macrophages in C57BL/6 mice. Shock 22:248–253
Vega VL, Charles W, Crotty Alexander LE (2011) Rescuing of deficient killing and phagocytic activities of macrophages derived from non-obese diabetic mice by treatment with geldanamycin or heat shock: potential clinical implications. Cell Stress Chaperones 16:573–581
Crotty Alexander LE, Akong-Moore K, Feldstein S, Johansson P, Nguyen A, McEachern EK, Nicatia S, Cowburn AS, Olson J, Cho JY et al (2013) Myeloid cell HIF-1alpha regulates asthma airway resistance and eosinophil function. J Mol Med 91:637–644
Paidas CN, Mooney ML, Theodorakis NG, De Maio A (2002) Accelerated recovery after endotoxic challenge in heat shock-pretreated mice. Am J Physiol Regul Integr Comp Physiol 282:R1374–1381
Cramer T, Yamanishi Y, Clausen BE, Forster I, Pawlinski R, Mackman N, Haase VH, Jaenisch R, Corr M, Nizet V et al (2003) HIF-1alpha is essential for myeloid cell-mediated inflammation. Cell 112:645–657
Chow CW, Downey GP, Grinstein S (2004) Measurements of phagocytosis and phagosomal maturation. Current protocols in cell biology. 22:15.7:15.7.1–15.7.33
Crotty Alexander LE, Maisey HC, Timmer AM, Rooijakkers SH, Gallo RL, von Kockritz-Blickwede M, Nizet V (2010) M1T1 group A streptococcal pili promote epithelial colonization but diminish systemic virulence through neutrophil extracellular entrapment. J Mol Med 88:371–381
Liebl D, Griffiths G (2009) Transient assembly of F-actin by phagosomes delays phagosome fusion with lysosomes in cargo-overloaded macrophages. J Cell Sci 122:2935–2945
Chow OA, von Kockritz-Blickwede M, Bright AT, Hensler ME, Zinkernagel AS, Cogen AL, Gallo RL, Monestier M, Wang Y, Glass CK et al (2010) Statins enhance formation of phagocyte extracellular traps. Cell Host Microbe 8:445–454
Aulik NA, Hellenbrand KM, Czuprynski CJ (2012) Mannheimia haemolytica and its leukotoxin cause macrophage extracellular trap formation by bovine macrophages. Infect Immun 80:1923–1933
Mohanan S, Horibata S, McElwee JL, Dannenberg AJ, Coonrod SA (2013) Identification of macrophage extracellular trap-like structures in mammary gland adipose tissue: a preliminary study. Front Immunol 4:67
Wong KW, Jacobs WR Jr (2013) Mycobacterium tuberculosis exploits human interferon gamma to stimulate macrophage extracellular trap formation and necrosis. J Infect Dis 208:109–119
Hellenbrand KM, Forsythe KM, Rivera-Rivas JJ, Czuprynski CJ, Aulik NA (2013) Histophilus somni causes extracellular trap formation by bovine neutrophils and macrophages. Microb Pathog 54:67–75
Goldmann O, Medina E (2012) The expanding world of extracellular traps: not only neutrophils but much more. Front Immunol 3:420
von Kockritz-Blickwede M, Nizet V (2009) Innate immunity turned inside-out: antimicrobial defense by phagocyte extracellular traps. J Mol Med 87:775–783
Murray PJ (2006) Understanding and exploiting the endogenous interleukin-10/STAT3-mediated anti-inflammatory response. Curr Opin Pharmacol 6:379–386
Murray PJ (2005) The primary mechanism of the IL-10-regulated antiinflammatory response is to selectively inhibit transcription. Proc Natl Acad Sci U S A 102:8686–8691
Nakanishi Y, Nakatsuji M, Seno H, Ishizu S, Akitake-Kawano R, Kanda K, Ueo T, Komekado H, Kawada M, Minami M et al (2011) COX-2 inhibition alters the phenotype of tumor-associated macrophages from M2 to M1 in ApcMin/+mouse polyps. Carcinogenesis 32:1333–1339
Nair MG, Cochrane DW, Allen JE (2003) Macrophages in chronic type 2 inflammation have a novel phenotype characterized by the abundant expression of Ym1 and Fizz1 that can be partly replicated in vitro. Immunol Lett 85:173–180
Keshari RS, Jyoti A, Dubey M, Kothari N, Kohli M, Bogra J, Barthwal MK, Dikshit M (2012) Cytokines induced neutrophil extracellular traps formation: implication for the inflammatory disease condition. PLoS One 7:e48111
Saitoh T, Komano J, Saitoh Y, Misawa T, Takahama M, Kozaki T, Uehata T, Iwasaki H, Omori H, Yamaoka S et al (2012) Neutrophil extracellular traps mediate a host defense response to human immunodeficiency virus-1. Cell Host Microbe 12:109–116
Neeli I, Dwivedi N, Khan S, Radic M (2009) Regulation of extracellular chromatin release from neutrophils. J Innate Immun 1:194–201
Zasloff M (2002) Antimicrobial peptides of multicellular organisms. Nature 415:389–395
Cunliffe RN, Mahida YR (2004) Expression and regulation of antimicrobial peptides in the gastrointestinal tract. J Leukoc Biol 75:49–58
Hancock RE (2001) Cationic peptides: effectors in innate immunity and novel antimicrobials. Lancet Infect Dis 1:156–164
Acknowledgments
We thank Molly Wofford for her editorial assistance. We thank Elisa McEachern and Matthew Lyes for their intellectual and experimental contributions. This work was supported through a Veterans Affairs Career Development Award (CDA)-2, BX-10-014 (PI, Laura E. Crotty Alexander), The Hartwell Foundation Biomedical Research Fellowship (Laura E. Crotty Alexander), University of California San Diego Academic Senate Grant (PI, Virginia L. Vega), and GM R01 098455 and GM R25 083275 grants (PI, Antonio De Maio).
Conflict of interest
The authors have no financial conflicts of interest.
Authors’ contribution
LECA, VLV, and JHW designed all of the experiments. LECA, VLV, WC, and JHW ran all of the experiments. LECA, VLV, JHW, VN, and ADM analyzed and interpreted all of the data and wrote the manuscript.
Author information
Authors and Affiliations
Corresponding author
Additional information
V. L. Vega and L. E. Crotty Alexander contributed equally to this work
Electronic supplementary material
Below is the link to the electronic supplementary material.
ESM 1
(PDF 251 kb)
Rights and permissions
About this article
Cite this article
Vega, V.L., Crotty Alexander, L.E., Charles, W. et al. Activation of the stress response in macrophages alters the M1/M2 balance by enhancing bacterial killing and IL-10 expression. J Mol Med 92, 1305–1317 (2014). https://doi.org/10.1007/s00109-014-1201-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00109-014-1201-y