Abstract
Purpose
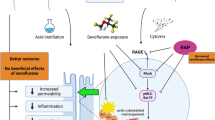
Gamma-aminobutyric acid (GABA) is the major inhibitory neurotransmitter through activation of GABA receptors. Volatile anesthetics activate type-A (GABAA) receptors resulting in inhibition of synaptic transmission. Lung epithelial cells have been recently found to express GABAA receptors that exert anti-inflammatory properties. We hypothesized that the volatile anesthetic sevoflurane (SEVO) attenuates lung inflammation through activation of lung epithelial GABAA receptors.
Methods
Sprague–Dawley rats were anesthetized with SEVO or ketamine/xylazine (KX). Acute lung inflammation was induced by intratracheal instillation of endotoxin, followed by mechanical ventilation for 4 h at a tidal volume of 15 mL/kg without positive end-expiratory pressure (two-hit lung injury model). To examine the specific effects of GABA, healthy human lung epithelial cells (BEAS-2B) were challenged with endotoxin in the presence and absence of GABA with and without addition of the GABAA receptor antagonist picrotoxin.
Results
Anesthesia with SEVO improved oxygenation and reduced pulmonary cytokine responses compared to KX. This phenomenon was associated with increased expression of the π subunit of GABAA receptors and glutamic acid decarboxylase (GAD). The endotoxin-induced cytokine release from BEAS-2B cells was attenuated by the treatment with GABA, which was reversed by the administration of picrotoxin.
Conclusion
Anesthesia with SEVO suppresses pulmonary inflammation and thus protects the lung from the two-hit injury. The anti-inflammatory effect of SEVO is likely due to activation of pulmonary GABAA signaling pathways.
Similar content being viewed by others
Introduction
Acute lung injury (ALI) is a major challenge in critical illness that is associated with high mortality [1]. The majority of patients suffering from ALI require mechanical ventilation for life support [2, 3]. However, mechanical ventilation per se bears the risk of inducing and worsening pulmonary dysfunction described as ventilator-induced lung injury (VILI) [4]. An important approach to manage patients with ALI is to reduce pulmonary and systemic inflammatory responses that may have played an important role in inducing multiple distal organ dysfunction [1, 2].
Low tidal volume ventilation has been considered as a protective ventilator strategy [2], but it may not suit all patients with respiratory failure [5]. Volatile anesthetics have been recently shown to exert anti-inflammatory effects in several experimental and clinical settings [6–8], which may be beneficial in the context of VILI. The use of sevoflurane (SEVO) can increase expression of IκB while decreasing NF-κB nuclear translocation following challenge with tumor necrosis factor α (TNF-α) in human monocytes [8]. The administration of SEVO improved gas exchange and attenuated lung injury after endotracheal installation of endotoxin in rats [6]. Anesthesia with SEVO has been shown to decrease the production of inflammatory cytokines including TNF-α, interleukin-6 (IL-6), and IL-8 in lung lavage fluids and reduced postoperative adverse events in patients under thoracic surgery [7]. However, the mechanisms by which SEVO exerts the anti-inflammatory effects remain unclear.
It is known that volatile anesthetics such as SEVO activate type-A gamma-aminobutyric acid (GABAA) receptors resulting in inhibition of synaptic transmission in neurons [9, 10]. GABA synthesized from glutamate by decarboxylation via the enzymatic activity of glutamic acid decarboxylase (GAD) produces fast synaptic inhibition in neurons through activating GABAA receptors, a GABA-gated anion channel. In addition to its conventional role in synaptic transmission, GABAA receptors also exert novel anti-inflammatory properties in the central nervous system [11] and in peripheral immune cells [12].
It is interesting that recent studies have demonstrated that GABAA receptors are also expressed in lung airway and alveolar epithelial cells [13–16]. However, their local role in response to inhalation of SEVO remains to be investigated in the context of ALI. We thus hypothesized that anesthesia with SEVO attenuates pulmonary inflammatory response through activation of GABAA receptors in lung epithelial cells. To test this hypothesis we examined the effects of SEVO on the expression of GABAA receptors and cytokine responses in a rat model of ALI, and the specific effects of GABA on cytokine responses in vitro in human lung epithelial cells.
Materials and methods
Anesthesia and mechanical ventilation
The study was approved by the institutional Animal Care Committee (ACC948) of St. Michael’s Hospital. Thirty-four Sprague–Dawley rats (250–350 g) were randomly assigned to receive anesthesia with either ketamine + xylazine (KX, n = 17) or sevoflurane (SEVO, n = 17). In the KX group, anesthesia was induced using ketamine at 80 mg/kg and xylazine at 8 mg/kg intraperitoneally, followed by continuous intravenous (i.v.) infusion of ketamine at 15 mg/kg/h and xylazine at 3 mg/kg/h. In the SEVO group, anesthesia was induced by 3.5 vol % SEVO in a closed chamber and maintained with 2.6 vol %. These doses of anesthetics were chosen on the basis of pilot experiments targeting similar mean arterial blood pressure (MAP) and comparable depth of anesthesia defined by no reaction to toe pinches prior to neuromuscular blockade. Tracheotomy was performed followed by intratracheal intubation with a 14G angiocatheter. Neuromuscular blockade was achieved by i.v. infusion of pancuronium at 0.5 mg/kg/h.
The following initial settings were applied using a rodent ventilator (Harvard 683): inspired oxygen fraction (FIO2) of 0.40, positive end-expiratory pressure (PEEP) of 5 cmH2O, tidal volume (VT) of 6 mL/kg, and respiratory rate (RR) adjusted to keep arterial partial pressure of CO2 (PaCO2) between 35 and 45 mmHg. The right carotid artery was cannulated (0.58 mm ID polyethylene tube) for continuous blood pressure monitoring. Intravenous infusion of lactated Ringer’s solution at 3 mL/kg/h was administered through the tail vein in all animals. Rectal temperature was maintained at 37 ± 1 °C using a heating blanket.
Two-hit model of ALI
All animals received intratracheal instillation of endotoxin at 5 mg/kg (LPS, Escherichia coli serotype 055:B5, Sigma-Aldrich). Thirty minutes later, mechanical ventilation was switched to high V T at 15 mL/kg and PEEP = 0 cmH2O for 4 h.
Measurements
Mean arterial blood pressure was monitored in a real-time fashion. Arterial blood gases (PaO2, PaCO2) were recorded hourly throughout the experiments.
Bronchoalveolar lavage (BAL) was performed in the left lung by using cold normal saline upon completion of the experiments. The BAL fluid was centrifuged at 4 °C and 1,200×g for 10 min and the supernatant was stored at −80 °C for further analysis.
Lung wet/dry ratio (WD ratio) was obtained after excision of the right lung and drying at 60 °C for 72 h.
The concentrations of glucose and lactate in blood were measured (Radiometer ABL 700 blood gas analyzer) at the end of the study.
Levels of intercellular adhesion molecule 1 (ICAM-1) and multiple cytokines including interleukin-1β (IL-1β), IL-2, IL-4, IL-10, IL-12, keratinocyte chemoattractant (KC), monocyte chemotactic protein-1 (MCP-1), macrophage inflammatory protein-1 alpha (MIP-1α), and tumor necrosis factor-alpha (TNF-α) were measured using species-specific multiplex cytokine assays (Bio-Rad) as previously described [17].
Basal expression of GAD (GAD65/67 antibody, Abcam, Inc., Cambridge, MA) and GABAA receptors (GABAA receptor alpha 2 antibody, Abcam, Inc.) was detected by immunohistochemistry in rats killed by cervical dislocation without undergoing the experimental protocol to serve as healthy controls. The methods have been previously described by the authors [15]. GAD expression was also assessed by Western blot (GAD65/67 antibody, Abcam, Inc.) analysis as previously described [15].
Cell culture and treatment
Human bronchial epithelial cells (BEAS-2B, ATTC) were cultured in full confluence and incubated with GABA (100 nM) alone or GABA + picrotoxin, a GABAA receptor antagonist (PTX, 50 nM) for 10 min, followed by stimulation with LPS at 100 ng/mL (Escherichia coli serotype 055:B5, Sigma-Aldrich) for 4 h. This dose of LPS has been previously used for induction of inflammatory responses [18].
Statistical analysis
Data are presented as mean and standard deviation. Student’s t test for unpaired samples was used to compare differences among groups at time zero and for postmortem analysis. Repeated measurements over time were analyzed with two-way analysis of variance for repeated measurements and adjusted with the Bonferroni post test. Statistical significance was considered if p < 0.05.
Results
Body weight was similar in all animals. The amount of fluid infused was not different in both groups (11.3 ± 0.7 mL in SEVO group vs. 12.5 ± 1.4 mL in KX group). Although the glucose level was slightly higher in the SEVO group than in the KX group (8.59 ± 0.57 mmol/L vs. 7.83 ± 0.18 mmol/L) the difference did not reach statistical significance. However, a lower level of lactate in blood was observed in the SEVO group than the KX group (2.26 ± 0.23 mmol/L vs. 3.35 ± 0.45 mmol/L, p < 0.05).
Hemodynamics and gas exchange
Mean arterial blood pressure and PaCO2 showed a similar time course in all animals (Fig. 1a, b respectively). Partial pressure of oxygen decreased significantly starting 2 h after high V T ventilation in the KX group as compared to the SEVO group (Fig. 1c). The decreased level of PaO2 was associated with an increase in lung wet/dry ratio suggesting greater lung permeability in the KX group (Fig. 1d).
a Mean arterial blood pressure (MAP), b arterial partial pressure of carbon dioxide (PaCO2), and c arterial partial pressure of oxygen (PaO2) in animals anesthetized with ketamine/xylazine (KX) or sevoflurane (SEVO) over time. d Lung wet/dry weight ratio was determined at the end of 4-h mechanical ventilation started 30 min after LPS administration. N = 17 per group
Pulmonary inflammatory response
The total leukocyte count in BAL fluid was significantly lower in the SEVO group compared to the KX group (0.85 ± 0.04 × 106 vs. 1.03 ± 0.05 × 106, p < 0.05). Although there was a trend of decrease in the percentage of polymorphonuclear cells over the total leukocytes (55 ± 5 vs. 69 ± 6 %), the difference did not reach statistical significance. The cytokine profile in BAL fluid showed lower levels of TNF-α, MIP-1α, IL-1β, KC, MCP-1, and ICAM-1 under anesthesia with SEVO compared to that under anesthesia with KX (Fig. 2).
Cytokine and ICAM-1 responses in animals anesthetized with ketamine/xylazine (KX) or sevoflurane (SEVO). Bronchoalveolar lavage (BAL) fluid was obtained at the end of 4-h mechanical ventilation started 30 min after LPS intratracheal administration. a Tumor necrosis factor-alpha (TNF-α), b macrophage inflammatory protein-1 alpha (MIP-1α), c interleukin-1 beta (IL-1β), d keratinocyte growth factor (KC), e monocyte chemotactic protein-1 (MCP-1), and f intracellular adhesion molecule-1 (ICAM-1). N = 17 per group
Immunohistochemistry
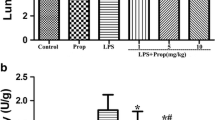
Immunohistochemistry showed a basal expression of GAD and GABAARα unit colocalized with lung epithelium stained with surfactant protein C of healthy rats (Fig. 3a). Western blot assay showed a higher protein level of GAD in the SEVO group than in the KX group (Fig. 3b).
Lung expression of GAD and GABAAR receptor. a Immunohistochemistry staining for the epithelial marker surfactant protein C (SPC; green), and GAD (red), GABAAR (red) and their overlay (orange) in healthy rat lungs. b Western blot for detection of GAD in animals anesthetized with KX or SEVO at the end of 4-h mechanical ventilation started 30 min after LPS intratracheal administration. Average expression of GAD over β-actin was from five experiments
In vitro BEAS-2B cell experiments
To investigate the specific effects of GABA in lung epithelial cells, human BEAS-2B cells were stimulated with LPS followed by treatment with GABA, PTX, or GABA + PTX. We first confirmed that the dose of PTX used did not induce cytotoxicity as reflected by a constant LDH level before and after PTX administration [19]; thus, cell viability was no affected (data not shown). Interleukin-1β was significantly reduced with GABA and GABA + PTX compared to control and PTX alone group (Fig. 4a). Interleukin-2 was significantly decreased with GABA and PTX compared to GABA + PTX (Fig. 4b). The concentrations of IL-8 and IL-10 decreased significantly with GABA, which was reversed by administration of PTX (Fig. 4c, d respectively).
Cytokine responses in BEAS-2B cells. Concentration of a interleukin-1β, b interleukin-2, c interleukin-8, and c interleukin-10 measured in cell culture supernatants of human bronchial epithelial cells (BEAS-2B) stimulated with LPS (control) followed by incubation with gamma-aminobutyric acid (GABA), picrotoxin (PTX), or GABA + PTX for 8 h. N = 5 experiments per group
Discussion
We demonstrate that anesthesia with SEVO improves oxygenation and reduced pulmonary cytokine responses associated with increased expression of GABAA as compared to anesthesia with KX. These results suggest that the activation of GABAA receptors may play a role in the lung-protective effect seen with SEVO.
An established two-hit model was chosen for its clinical relevance in that primary lung inflammation/injury was followed by mechanical ventilation as a treatment [6]. Since the use of either ketamine or xylazine alone is not recommended, a regime of the combination is commonly used for animal anesthesia [20]. We examined two regimes of anesthesia by choosing SEVO and KX in the present study. To avoid possible interference and/or crossover effects between the SEVO and KX, the same anesthetic regime was used for both induction and maintenance. Because the two anesthetic regimes function through distinct mechanisms of action, this would help us understand the possible signaling pathways responsible for their effects. SEVO acts mainly via agonistic effects on GABAA receptors. Ketamine interacts mainly with the NMDA-subtype glutamate receptor, but at high, fully anesthetic level doses, it binds to opioid μ receptors and sigma receptors [21–23].
In comparison with SEVO, ketamine has minor effects by selectively acting on α6 and δ subunits of GABA receptors [22]. The majority of literature suggested that ketamine exerts antagonistic action at the GABAA receptor complex [24–26]. In particular, ketamine has been reported to decrease the GAD67 isoform [27]. Our results are in agreement with these previous studies [25–27]. It is noted that subanesthetic doses of ketamine reportedly inhibit tonic convulsions induced by the GABAA receptor antagonist bicuculline, and the latter antagonized ketamine anesthesia [28]. However, the suggested agonistic effects of ketamine on GABAA are yet to be examined specifically under in vitro and in vivo conditions. Xylazine is a clonidine analogue acting on presynaptic and postsynaptic receptors of the central and peripheral nervous systems as an α2-adrenergic agonist that is used primarily for sedation, anesthesia, analgesia, and muscle relaxation in animal models [29]. Similar drugs such as clonidine and dexmedetomidine are increasingly used in clinical anesthesia and critical care [30]. The different pharmacological actions of the anesthetics used in this study may explain their distinct anti-inflammatory properties. In addition, paralysis was applied by administration of a given dose of pancuronium in all animals to achieve animal–ventilator synchrony in order to minimize signal to noise ratio and to enhance reproducibility of the experiments. It is therefore evident that the paralysis was part of the anesthesia regimes used in the present study.
Various inflammatory mediators including the cytokines TNF-α and IL-1β, chemokines, and ICAM-1 have been shown to act as effector molecules in the disruption of the epithelial and endothelial barrier during mechanical ventilation [31, 32]. We observe that the administration of SEVO attenuated the production of the inflammatory mediators in the lung and thus reduced lung permeability. Our results are in agreement with other studies showing anti-inflammatory effects of volatile anesthetics in a variety of in vivo and in vitro models. In an ischemia–reperfusion model of acute kidney injury, Lee et al. [33] reported direct anti-inflammatory and antinecrotic effects of SEVO by activation of prosurvival kinases and increase in de novo synthesis of heat shock protein 70. Boost et al. [8] demonstrated that isoflurane, acting also on GABAA receptors [34], attenuates the release of IL-8 and heme oxygenase 1 in human monocytic THP-1 cells in vitro through a mechanism by which the volatile anesthetic stabilizes the NF-κB inhibitory pathway.
Interleukin-10 was originally discovered as the cytokine synthesis inhibiting factor on the basis of its biological activity. It downregulates the expression of pro-inflammatory cytokines such as IL-1β, MHC class II antigens, and co-stimulatory molecules by upregulation of itself. In the present study, the administration of GABA attenuated the LPS-induced production of IL-1β and IL-10 in BEAS-2B cells. This phenomenon is consistent with previous reports showing that concentrations of IL-1β and IL-10 increased in response to LPS challenge to counterbalance the pro- and anti-inflammatory responses [35, 36].
A recent study by Faller and colleagues [37] reported that the administration of the volatile anesthetic isoflurane resulted in a reduction in lung damage, inflammation, and stress protein expression in a mouse model of VILI using a tidal volume of 12 mL/kg for 6 h. Our data are consistent with their observation despite that we use a two-hit model of ALI followed mechanical ventilation under the anesthesia with SEVO. Taken together, our results and the previous study [37] support the concept that volatile anesthetics exert anti-inflammatory effects protecting the lung from injury.
Volatile anesthetics produce anesthetic action primarily by binding to GABAA receptors in neurons of the central nervous system (CNS) [15]. Specifically, SEVO activates GABAA receptors in the CNS resulting in an inhibition of neuronal activities [9, 15]. We have previously discovered the existence of GAD and GABA receptors in human airway epithelial cells [15], and other investigators identified GABA receptors in alveolar epithelial type II cells [14]. In an ongoing study, we observed that volatile anesthetics including SEVO also enhance GABAA receptor-mediated anion current in pulmonary epithelial cells. In the present study, we further confirmed the presence of GAD and GABAA receptors both in rat airway and alveolar epithelial cells. We also demonstrate that anesthesia with SEVO results in an increase in expression of GAD and GABAA receptors in the lung compared with KX. We speculate that an increase in GAD expression after SEVO administration may be due to a positive feedback mechanism as a result of the binding between SEVO and GABAA receptors.
The concentrations of cytokines were lower and the GAD expression was higher in the SEVO group than in the KX group under in vivo conditions. These observations suggest that SEVO exerts anti-inflammatory properties partially by upregulation of GABA receptors. This concept was further supported by the in vitro lung epithelial cell studies where LPS-induced cytokine responses were attenuated in the presence of GABA, which was reversed by the administration of picrotoxin. Furthermore, it has been reported that an increase in surface levels of GABAA receptors requires the activity of phosphoinositide 3-kinase (PI3K) and protein kinase C [38]. This is in accord with a recent study reporting that a mechanism by which isoflurane reduced VILI was through increasing phosphorylation of Akt protein, since the inhibition of phosphoinositide 3-kinase/Akt signaling prior to mechanical ventilation completely reversed the lung-protective effects of isoflurane in mice [37].
It is noteworthy that anesthesia with SEVO or KX may result in hyperglycemia in rats [39, 40]. Clinical and experimental data suggest that hyperglycemia is protective against the development of ALI/ARDS [41]. We observe that the blood glucose level was higher in the SEVO group than in the KX group although the difference did not reach statistical significance. However, whether a different effect on glycemia between SEVO and KX might provide an additional pathway by which SEVO exerts a protective effect remains to be further investigated.
There are several limitations in the study. (1) The experimental double-hit model used may not reflect the complex clinical scenario seen in patients with ALI/ARDS. (2) The involvement of GABAA receptors was the focus of the study; whether other mechanisms are also responsible for the protective effects of SEVO remains to be elucidated. (3) As the study design compares the modulation of pulmonary inflammatory responses during mechanical ventilation by two different anesthesia regimens, it is impossible to conclude whether the difference is due to the protective effects of one or the detrimental effects of the other single agent. (4) We focused the investigation on SEVO in the present study; further studies using other volatile (e.g. desflurane or isoflurane) or intravenous (i.e. propofol or midazolam) anesthetics are warranted.
In summary, we demonstrate that anesthesia with sevoflurane can improve oxygenation and reduce pulmonary cytokine responses as compared to ketamine/xylazine. The protective effects of sevoflurane appear to be associated with its agonistic effects at GABAA receptors.
References
Phua J, Badia JR, Adhikari NK, Friedrich JO, Fowler RA, Singh JM, Scales DC, Stather DR, Li A, Jones A, Gattas DJ, Hallett D, Tomlinson G, Stewart TE, Ferguson ND (2009) Has mortality from acute respiratory distress syndrome decreased over time? A systematic review. Am J Respir Crit Care Med 179:220–227
The Acute Respiratory Distress Syndrome Network (2000) Ventilation with lower tidal volumes as compared with traditional tidal volumes for acute lung injury and the acute respiratory distress syndrome. N Engl J Med 342:1301–1308
Brun-Buisson C, Minelli C, Bertolini G, Brazzi L, Pimentel J, Lewandowski K, Bion J, Romand J, Villar J, Thorsteinsson A, Damas P, Armaganidis A, Lemaire F, Alive Study Group (2004) Epidemiology and outcome of acute lung injury in European intensive care units. Results from the ALIVE study. Intensive Care Med 30:51–61
Tremblay L, Valenza F, Ribeiro SP, Li J, Slutsky AS (1997) Injurious ventilatory strategies increase cytokines and c-fos m-RNA expression in an isolated rat lung model 4. J Clin Invest 99:944–952
Malhotra A (2007) Low-tidal-volume ventilation in the acute respiratory distress syndrome. N Engl J Med 357:1113–1120
Voigtsberger S, Lachmann RA, Leutert AC, Schlapfer M, Booy C, Reyes L, Urner M, Schild J, Schimmer RC, Beck-Schimmer B (2009) Sevoflurane ameliorates gas exchange and attenuates lung damage in experimental lipopolysaccharide-induced lung injury. Anesthesiology 111:1238–1248
De Conno E, Steurer MP, Wittlinger M, Zalunardo MP, Weder W, Schneiter D, Schimmer RC, Klaghofer R, Neff TA, Schmid ER, Spahn DR, Z’Graggen BR, Urner M, Beck-Schimmer B (2009) Anesthetic-induced improvement of the inflammatory response to one-lung ventilation. Anesthesiology 110:1316–1326
Boost KA, Leipold T, Scheiermann P, Hoegl S, Sadik CD, Hofstetter C, Zwissler B (2009) Sevoflurane and isoflurane decrease TNF-alpha-induced gene expression in human monocytic THP-1 cells: potential role of intracellular I kappa B alpha regulation. Int J Mol Med 23:665–671
Hirota K, Roth SH (1997) Sevoflurane modulates both GABAA and GABAB receptors in area CA1 of rat hippocampus. Br J Anaesth 78:60–65
Sebel LE, Richardson JE, Singh SP, Bell SV, Jenkins A (2006) Additive effects of sevoflurane and propofol on gamma-aminobutyric acid receptor function. Anesthesiology 104:1176–1183
Bhat R, Axtell R, Mitra A, Miranda M, Lock C, Tsien RW, Steinman L (2010) Inhibitory role for GABA in autoimmune inflammation. Proc Natl Acad Sci USA 107:2580–2585
Duthey B, Hubner A, Diehl S, Boehncke S, Pfeffer J, Boehncke WH (2010) Anti-inflammatory effects of the GABAB receptor agonist baclofen in allergic contact dermatitis. Exp Dermatol 19:661–666
Jin N, Kolliputi N, Gou D, Weng T, Liu L (2006) A novel function of ionotropic gamma-aminobutyric acid receptors involving alveolar fluid homeostasis. J Biol Chem 281:36012–36020
Jin N, Narasaraju T, Kolliputi N, Chen J, Liu L (2005) Differential expression of GABAA receptor pi subunit in cultured rat alveolar epithelial cells. Cell Tissue Res 321:173–183
Xiang YY, Wang S, Liu M, Hirota JA, Li J, Ju W, Fan Y, Kelly MM, Ye B, Orser B, O’Byrne PM, Inman MD, Yang X, Lu WY (2007) A GABAergic system in airway epithelium is essential for mucus overproduction in asthma. Nat Med 13:862–867
Mizuta K, Osawa Y, Mizuta F, Xu D, Emala CW (2008) Functional expression of GABAB receptors in airway epithelium. Am J Respir Cell Mol Biol 39:296–304
Voglis S, Quinn K, Tullis E, Liu M, Henriques M, Zubrinich C, Penuelas O, Chan H, Silverman F, Cherepanov V, Orzech N, Khine AA, Cantin A, Slutsky AS, Downey GP, Zhang H (2009) Human neutrophil peptides and phagocytic deficiency in bronchiectatic lungs. Am J Respir Crit Care Med 180:159–166
Zhang H, Kim YK, Govindarajan A, Baba A, Binnie M, Marco Ranieri V, Liu M, Slutsky AS (1999) Effect of adrenoreceptors on endotoxin-induced cytokines and lipid peroxidation in lung explants. Am J Respir Crit Care Med 160:1703–1710
Racher AJ, Looby D, Griffiths JB (1990) Use of lactate dehydrogenase release to assess changes in culture viability. Cytotechnology 3:301–307
Green CJ, Knight J, Precious S, Simpkin S (1981) Ketamine alone and combined with diazepam or xylazine in laboratory animals: a 10 year experience. Lab Anim 15:163–170
Narita M, Yoshizawa K, Aoki K, Takagi M, Miyatake M, Suzuki T (2001) A putative sigma1 receptor antagonist NE-100 attenuates the discriminative stimulus effects of ketamine in rats. Addict Biol 6:373–376
Hevers W, Hadley SH, Luddens H, Amin J (2008) Ketamine, but not phencyclidine, selectively modulates cerebellar GABAA receptors containing alpha6 and delta subunits. J Neurosci 28:5383–5393
Hirota K, Sikand KS, Lambert DG (1999) Interaction of ketamine with mu2 opioid receptors in SH-SY5Y human neuroblastoma cells. J Anesth 13:107–109
Kounenis G, Koutsoviti-Papadopoulou M, Elezoglou V (1995) Ketamine may modify intestinal motility by acting at GABAA-receptor complex; an in vitro study on the guinea pig intestine. Pharmacol Res 31:337–340
Vutskits L, Gascon E, Potter G, Tassonyi E, Kiss JZ (2007) Low concentrations of ketamine initiate dendritic atrophy of differentiated GABAergic neurons in culture. Toxicology 234:216–226
Sonner JM, Zhang Y, Stabernack C, Abaigar W, Xing Y, Laster MJ (2003) GABAA receptor blockade antagonizes the immobilizing action of propofol but not ketamine or isoflurane in a dose-related manner. Anesth Analg 96:706–712
Zhang Y, Behrens MM, Lisman JE (2008) Prolonged exposure to NMDAR antagonist suppresses inhibitory synaptic transmission in prefrontal cortex. J Neurophysiol 100:959–965
Irifune M, Sato T, Kamata Y, Nishikawa T, Dohi T, Kawahara M (2000) Evidence for GABAA receptor agonistic properties of ketamine: convulsive and anaesthetic behavioural models in mice. Anesth Analg 91:230–236
Garcia-Villar R, Toutain PL, Alvinerie M, Ruckebusch Y (1981) The pharmacokinetics of xylazine hydrochloride: an interspecific study. J Vet Pharmacol Ther 4:87–92
Riker RR, Shehabi Y, Bokesch PM, Ceraso D, Wisemandle W, Koura F, Whitten P, Margolis BD, Byrne DW, Ely EW, Rocha MG (2009) Dexmedetomidine vs midazolam for sedation of critically ill patients: a randomized trial. JAMA 301:489–499
Bruewer M, Luegering A, Kucharzik T, Parkos CA, Madara JL, Hopkins AM, Nusrat A (2003) Proinflammatory cytokines disrupt epithelial barrier function by apoptosis-independent mechanisms. J Immunol 171:6164–6172
Choi H, Fleming NW, Serikov VB (2007) Contact activation via ICAM-1 induces changes in airway epithelial permeability in vitro. Immunol Invest 36:59–72
Lee HT, Kim M, Jan M, Emala CW (2006) Anti-inflammatory and antinecrotic effects of the volatile anaesthetic sevoflurane in kidney proximal tubule cells. Am J Physiol Renal Physiol 291:F67–F78
Jia F, Yue M, Chandra D, Homanics GE, Goldstein PA, Harrison NL (2008) Isoflurane is a potent modulator of extrasynaptic GABAA receptors in the thalamus. J Pharmacol Exp Ther 324:1127–1135
Erickson MA, Banks WA (2011) Cytokine and chemokine responses in serum and brain after single and repeated injections of lipopolysaccharide: multiplex quantification with path analysis. Brain Behav Immun 25:1637–1648
Ward JL, Harting MT, Cox CS Jr, Mercer DW (2011) Effects of ketamine on endotoxin and traumatic brain injury induced cytokine production in the rat. J Trauma 70:1471–1479
Faller S, Strosing KM, Ryter SW, Buerkle H, Loop T, Schmidt R, Hoetzel A (2012) The volatile anaesthetic isoflurane prevents ventilator-induced lung injury via phosphoinositide 3-kinase/Akt signaling in mice. Anesth Analg 114:747–756
Porcher C, Hatchett C, Longbottom RE, McAinch K, Sihra TS, Moss SJ, Thomson AM, Jovanovic JN (2011) Positive feedback regulation between gamma-aminobutyric acid type A (GABAA) receptor signaling and brain-derived neurotrophic factor (BDNF) release in developing neurons. J Biol Chem 286:21667–21677
Kaufman DA (2009) Time-dependent behavioral recovery after sepsis in rats. Intensive Care Med 35:576; author reply 577
Kitamura T, Ogawa M, Kawamura G, Sato K, Yamada Y (2009) The effects of sevoflurane and propofol on glucose metabolism under aerobic conditions in fed rats. Anesth Analg 109:1479–1485
Honiden S, Gong MN (2009) Diabetes, insulin, and development of acute lung injury. Crit Care Med 37:2455–2464
Acknowledgments
The authors are indebted to Julie Khang, BSc for technical assistance. The study was supported by Canadian Institutes of Health Research (CIHR) grants to WYL, Arthur S. Slutsky, and Haibo Zhang, Ontario Thoracic Society (OTS) Grant-in-Aid and McLaughlin Foundation to Haibo Zhang. Spyridon Fortis was supported by the Alexander S. Onassis Public Benefit Foundation. Peter M. Spieth was supported by the German Research Foundation (DFG SP 1222/3-1). Peter M. Spieth is a recipient of the University of Toronto Eli Lilly Critical Care Fellowship Award.
Author information
Authors and Affiliations
Corresponding author
Additional information
S. Fortis and P. M. Spieth contributed equally to the work.
Rights and permissions
About this article
Cite this article
Fortis, S., Spieth, P.M., Lu, WY. et al. Effects of anesthetic regimes on inflammatory responses in a rat model of acute lung injury. Intensive Care Med 38, 1548–1555 (2012). https://doi.org/10.1007/s00134-012-2610-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00134-012-2610-4