Abstract
Background
It is believed that increased intracranial pressure immediately after subarachnoid hemorrhage (SAH) causes extensive brain ischemia and results in worsening clinical status. Arterial flow to the cerebral surfaces is clinically well maintained during clipping surgery regardless of the severity of the World Federation of Neurological Societies grade after SAH. To explore what kinds of changes occur in the cortical microcirculation, not at the cerebral surface, we examined cortical microcirculation after SAH using two-photon laser scanning microscopy (TPLSM).
Methods
SAH was induced in mice with an endovascular perforation model. Following continuous injection of rhodamine 6G, velocities of labeled platelets and leukocytes and unlabeled red blood cells (RBCs) were measured in the cortical capillaries 60 min after SAH with a line-scan method using TPLSM, and the data were compared to a sham group and P-selectin monoclonal antibody-treated group.
Results
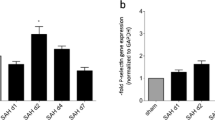
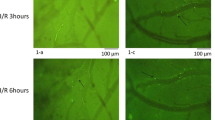
Velocities of leukocytes, platelets, and RBCs in capillaries decreased significantly 60 min after SAH. Rolling and adherent leukocytes suddenly prevented other blood cells from flowing in the capillaries. Flowing blood cells also decreased significantly in each capillary after SAH. This no-reflow phenomenon induced by plugging leukocytes was often observed in the SAH group but not in the sham group. The decreased velocities of blood cells were reversed by pretreatment with the monoclonal antibody of P-selection, an adhesion molecule expressed on the surfaces of both endothelial cells and platelets.
Conclusions
SAH caused sudden worsening of cortical microcirculation at the onset. Leukocyte plugging in capillaries is one of the reasons why cortical microcirculation is aggravated after SAH.





Similar content being viewed by others
References
Ames A III, Wright RL, Kowada M, Thurston JM, Majno G (1968) Cerebral ischemia II. The no-reflow phenomenon. Am J Pathol 52(2):437–453
Asano T, Sano K (1977) Pathogenetic role of no-reflow phenomenon in experimental subarachnoid hemorrhage in dogs. J Neurosurg 46(4):454–466
Bederson JB, Germano IM, Guarino L (1995) Cortical blood flow and cerebral perfusion pressure in a new noncraniotomy model of subarachnoid hemorrhage in the rat. Stroke 26(6):1086–1092
Coisne C, Faveeuw C, Delplace Y, Dehoyck L, Miller F, Cecchelli R, Dehouck L (2006) Differential expression of selectins by mouse brain capillary endothelial cells in vitro in response to distinct inflammatory stimuli. Neurosci Lett 392(3):216–220
del Zoppo GJ, Schmid-schoenbein GW, Mori E, Copeland BR, Chang C-M (1991) Polymorphonuclear leukocytes occlude capillaries following middle cerebral artery occlusion and reperfusion in baboons. Stroke 22(10):1276–1283
del Zoppo GJ, Hallenbeck JM (2000) Advances in the vascular pathophysiology of ischemic stroke. Thromb Res 98(3):V73–V81
Dirnagl U, Niwa K, Sixt G, Villringer A (1994) Cortical hypoperfusion after global forebrain ischemia in rats is not caused by microvascular leukocyte plugging. Stroke 25(5):1028–1038
Friedrich B, Mueller F, Feiler S, Schoeller K, Plesnila N (2012) Experimental subarachnoid hemorrhage causes early and long-lasting microarterial constriction and microthrombosis: an in-vivo microscopy study. J Cereb Blood Flow Metab 32(3):447–455
Friedrich V, Flores R, Muller A, Sehba FA (2010) Escape of intraluminal platelets into brain parenchyma after subarachnoid hemorrhage. Neuroscience 165(3):968–975
Germano A, d’Avella D, Cicciarello R, Hayes RL, Tomasello F (1992) Blood–brain barrier permeability changes after experimental subarachnoid hemorrhage. Neurosurgery 30(6):882–886
Girouard H, Iadecola C (2006) Neurovascular coupling in the normal brain and in hypertension, stroke, and Alzheimer disease. J Appl Physiol 100(1):328–335
Hayakawa T, Waltz AG (1977) Experimental subarachnoid hemorrhage from a middle cerebral artery. Neurologic deficits, intracranial pressures, blood pressures, and pulse rates. Stroke 8(4):421–426
Herz DA, Baez S, Shulman K (1975) Pial microcirculation in subarachnoid hemorrhage. Stroke 6(4):417–424
Huang J, Upadhyay UM, Tamargo RJ (2006) Inflammation in stroke and focal cerebral ischemia. Surg Neurol 66(3):232–245
Huang JY, Li LT, Wang H, Liu SS, Lu YM, Liao MH, Tao RR, Hong LJ, Fukunaga K, Chen Z, Wilcon CS, Lai EY, Han F (2014) In vivo two-photon fluorescence microscopy reveals disturbed cerebral capillary blood flow and increased susceptibility to ischemic insults in diabetic mice. CNS Neurosci Ther 20(9):816–822
Iadecola C, Nedergaard M (2007) Glial regulation of the cerebral microvasculature. Nat Neurosci 10(11):1369–1376
Ishikawa M, Stokes KY, Zhang JH, Nanda A, Granger DN (2004) Cerebral microvascular responses to hypercholesterolemia Role of NADPH oxidase and P-selectin. Circ Res 94(2):239–244
Ishikawa M, Vowinkel T, Stokes KY, Arumugan TV, Yilmaz G, Nanda A, Zhang JH, Granger DN (2005) CD40/CD40L signaling in mouse cerebral microvasculature after focal ischemia/.reperfusion. Circulation 111(13):1690–1696
Ishikawa M, Sekizuka E, Yamagchi N, Nakadate H, Terao S, Granger DN, Minamitani H (2007) Angiotensin II type 1 receptor signaling contributes to platelet-leukocyte-endothelial cell interactions in the cerebral microvasculature. Am J Physiol Heart Circ Physiol 292(5):H2306–H2315
Ishikawa M, Kusaka G, Yamaguchi N, Sekizuka E, Nakadate H, Minamitani H, Watanabe E (2009) Platelet and leukocyte adhesion in the microvasculature at the cerebral surface immediately after subarachnoid hemorrhage. Neurosurgery 64(3):546–554
Jerome SN, Dore M, Paulson JC, Smithi CW, Korthuis RJ (1994) P-selectin and ICAM-1-dependent adherence reactions: role in the genesis of postischemic no-reflow. Am J Physiol 266(4):H1316–H1321
Kamiya K, Kuyama H, Symon L (1983) An experimental study of the acute stage of subarachnoid hemorrhage. J Neurosurg 59(6):917–924
Kleinfeld D, Mitra PP, Helmchen F, Denk W (1998) Fluctuations and stimulus-induced changes in blood flow observed in individual capillaries in layers 2 through 4 of rat neocortex. Proc Natl Acad Sci U S A 95(26):15741–15746
Kusaka G, Ishikawa M, Nanda A, Neil Granger D, Zhang JH (2004) Signaling pathways for early brain injury after subarachnoid hemorrhage. J Cereb Brain Flow Metab 24(8):916–925
Li Z, Liang G, Ma T, Li J, Wang P, Liu L, Xue Y (2015) Blood- brain barrier permeability change and regulation mechanism after subarachnoid hemorrhage. Metab Brain Dis 30(2):597–603
Mori E, del Zoppo GJ, Chambers JD, Copeland BR, Arfors KE (1992) Inhibition of polymorphonuclear leukocyte adherence suppresses no-reflow after focal cerebral ischemia in baboons. Stroke 23(5):712–718
Morikawa T, Kajimura M, Nakamura T, Hishiki T, Nakanishi T, Yukutake Y, Nagahata Y, Ishikawa M, Hattori K, Takenouchi T, Takahashi T, Ishii I, Matsubara K, Kabe Y, Uchiyama S, Nagata E, Gadalla MM, Snyder SH, Suematsu M (2012) Hypoxic regulation of the cerebral microcirculation is mediated by a carbon monoxide-sensitive hydrogen sulfide pathway. PNAS 109(4):1293–1298
Nakamura T, Kajimura M, Morikawa T, Hattori K, Ishikawa M, Yukutake Y, Uchiyama S-I, Suematsu M (2011) Acute CO2-independent vasodilatation of penetrating and pre-capillary arterioles in mouse cerebral parenchyma upon hypoxia revealed by a thinned-skull window method. Acta Physiol 203(1):187–196
Pinsky DJ, Naka Y, Liao H, Oz MC, Wagner DD, Mayadas TN, Johnson RC, Hynes RO, Heath M, Lawson CA, Stem DM (1996) Hypoxia-induced exocytosis of endothelial cell Weibel-Palade bodies. A mechanism for rapid neutrophil recruitment after cardiac preservation. J Clin Invest 97(2):493–500
Schoeller K, Trinke A, Klopotowski M, Thal SC, Plesnila N, Trabold R, HamannGF S-ER, Zausinger S (2007) Characterization of microvascular basal lamina damage and blood–brain barrier dysfunction following subarachnoid hemorrhage in rats. Brain Res 1142:237–246
Sehba FA, Friedrich V, Makonnen G, Bederson JB (2007) Acute cerebral vascular injury after subarachnoid hemorrhage and its prevention by administration of a nitric oxide donor. J Neurosurg 106(2):321–329
Shih AY, Driscoll JD, Drew PJ, Nishimura N, Schaffer CB, Kleinfeld D (2012) Two-photon microscopy as a tool to study blood flow and neurovascular coupling in the rodent brain. J Cereb Blood Flow Metab 32(7):1277–1309
Sikora L, Johansson ACM, Rao SP, Hughes GK, Broide DH, Sriramarao P (2003) A murine model to study leukocyte rolling and intravascular trafficking in lung microvessels. Am J Pathol 162(6):2019–2028
Trojanowski T (1982) Blood–brain barrier changes after experimental subarachnoid haemorrhage. Acta Neurochir (Wien) 60(1–2):45–54
Trojanowski T (1982) Experimental subarachnoid haemorrhage. Part II: extravasation volume and dynamics of subarachnoid arterial bleeding in cats. Acta Neurochir 64(1–2):103–108
Trojanowski T (1984) Early effects of experimental arterial subarachnoid haemorrhage on the cerebral circulation. Part I: experimental subarachnoid haemorrhage in cat and its pathophysiological effects methods of regional cerebral blood flow measurement and evaluation of microcirculation. Acta Neurochir (Wien) 72(1–2):79–94
Trojanowski T (1984) Early effects of experimental arterial subarachnoid haemorrhage on the cerebral circulation. Part II: regional cerebral blood flow and cerebral microcirculation after experimental subarachnoid haemorrhage. Acta Neurochir (Wien) 72(3–4):241–259
Trojanowski T (2008) How intracranial aneurysm rupture damages the brain. Interv Neuroradiol 14(1):9–12
Villringer A, Dirnagl U, Them A, Schuerer L, Krombach F, Einhaeupl KM (1991) Imaging of leukocytes within the rat brain cortex in vivo. Microvasc Res 42(3):305–315
Yata K, Nishimura Y, Unekawa M, Tomita Y, Suzuki N, Tanaka T, Mizoguchi A, Tomimoto H (2014) In vivo imaging of the mouse neurovascular unit under chronic cerebral hypoperfusion. Stroke 45(12):3698–3703
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
The Japan Society for the Promotion of Science Grant-in-Aid provided financial support in the forms of Scientific Research (22591597, 25462233) funding for M.I. and Scientific Research (21500353, 24500448) funding for M.K. The Japan Science and Technology Agency provided financial support in the form of Exploratory Research for Advanced Technology funding for M.S.
Conflict of interest
None.
Ethical approval
All procedures performed in studies involving animals were in accordance with the ethical standards of the Keio University Animal Care and Use Committee (12070–2).
Additional information
Comments
The authors provided a very elegant study on the pathophysiology of the cortical microcirculation after subarachnoid hemorrhage (SAH) in a rodent model. They very clearly demonstrated that when a sudden increase of intracranial pressure (ICP) begins after SAH, blood cell velocities in the capillaries decrease significantly and “rolling” and adherent leukocytes plug capillaries, preventing other blood cells from flowing. According to the results here provided, this is the consequence of an ICP rise that determine the compression of capillaries and decrease of blood flow. This in turn causes cerebral ischemic damage and an inflammatory response. This study provides robust evidence about the subsistence of this pathophysiological event and interesting illustrations. Further studies to demonstrate the translational potential of these findings are warranted. In particular, it is true that an abrupt ICP rise is present after SAH. Nevertheless, this cortical dysfunction might be present only in severe SAH cases. I wonder whether it is the persistently elevated ICP, present in severe SAH grades, instead of an abrupt rise with a quick fall that plays a major role. An indication of the intensity and the duration of the ICP rise able to induce such microvessel paralysis would be desirable. Thus, the authors are invited to continue their studies and provide further data on this interesting issue.
Alfredo Conti
Messina, Italy
Rights and permissions
About this article
Cite this article
Ishikawa, M., Kajimura, M., Morikawa, T. et al. Leukocyte plugging and cortical capillary flow after subarachnoid hemorrhage. Acta Neurochir 158, 1057–1067 (2016). https://doi.org/10.1007/s00701-016-2792-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00701-016-2792-6