Abstract
Virus–specific antibodies protect individuals against a wide variety of viral infections1–7. To assess whether human immunodeficiency virus type 1 (HIV–1) envelope–specific antibodies confer resistance against primate lentivirus infections, we purified immunoglobulin (IgG) from chimpanzees infected with several different HIV–1 isolates, and used this for passive immunization of pig–tailed macaques. These monkeys were subsequently challenged intravenously with a chimeric simian–human immunodeficiency virus (SHIV) bearing an envelope glycoprotein derived form HIV–1DH12, a dual–tropic primary virus isolate. Here we show that anti–SHIV neutralizing activity, determined in vitro using an assay measuring loss of infectivity, is the absolute requirement for antibody–mediated protection in vivo. Using an assay that measures 100% neutralization, the titer in plasma for complete protection of the SHIV–challenged macaques was in the range of 1:5–1:8. The HIV–1–specific neutralizing antibodies studied are able to bind to native gp120 present on infectious virus particles. Administration of non–neutralizing anti–HIV IgG neither inhibited nor enhanced a subsequent SHIV infection.
Similar content being viewed by others
Main
Of the primate lentiviral vaccine approaches evaluated during the past decade, live attenuated vaccines have proven the most consistent for inducing resistance against subsequent virus challenges. However, because of concerns about the possible reversion to virulence and/or natural or induced fluctuations in immune function during the lifetime of the vaccinee that might lead to increased virus loads, other vaccine strategies are now being systematically assessed. Nonetheless, the delineation of protective mechanisms elicited by any vaccine against a primate lentiviral infection would be very useful for designing an effective prophylactic vaccine. Nonhuman primate model systems, such as HIV–1 infection in chimpanzees and SIV (simian immunodeficiency virus) or SHIV (simian–human chimeric immunodeficiency virus) infections in macaques have been widely used for this purpose8. Although live attenuated virus vaccines have been shown to confer resistance against HIV or SHIV by a mechanism(s) that does not involve neutralizing antibodies9,10,11, chimpanzee studies, including passive immunization experiments, correlated protection from HIV–1 infection with levels of neutralizing antibody12,13,14,15,16. These seemingly conflicting results indicate that a diversity of immunological mechanisms have the potential to protect animals from a retrovirus challenge. Here we have focused on antibody–mediated protection and have addressed a fundamental question relevant to the development of a prophylactic vaccine: Can high–titer antibody, directed against the HIV–1 envelope and capable of completely neutralizing an HIV infection in a tissue culture system, block the establishment of a SHIV infection in vivo after its passive transfer to macaque monkeys?
We studied chimpanzees that were infected with a variety of HIV–1 isolates and subsequently developed high–titer neutralizing antibodies. Ch 4750 had been simultaneously co–infected with three different clade B primary isolates, each representing a different host cell–tropic phenotype (HIV–1DH12, a T–cell line/macrophage dual–tropic primary virus isolate17; HIV–1DH20, T–tropic18; and HIV–1DH29, M–tropic18); Ch 1206 had been infected with HIV–1DH12 alone; Ch 911 had been infected with the T–tropic, clade B isolate, HIV–1IIIB (ref. 19); and Ch 73 was uninfected (Table 1 and Fig. 1a). IgG was prepared as described20 from these four chimpanzees and passively transferred to pig–tailed macaques. The macaques were subsequently challenged with the pathogenic MD14 derivative of SHIV–1DH12 (ref. 21)(Fig. 1b), a chimeric virus with envelope glycoproteins derived from HIV–1DH12, a dual–tropic primary virus isolate17. The ability of HIV–1DH12 to be neutralized was compared with that of several laboratory adapted, T cell–tropic HIV–1 isolates; two different human sera, capable of neutralizing HIV–1IIIB and HIV–1MN, failed to neutralize HIV–1DH12 (data not shown). The broadly neutralizing monoclonal antibody b12 (ref. 22) neutralized HIV–1DH12 in peripheral blood mononuclear cells (PBMC) at 4.7 μg/ml (as measured by 90% p24 reduction assay), a similar concentration to that required to neutralize other primary isolates (Ref. 22 and R.S., unpublished observation).
b, Genomic organization of the SHIVDH12 proviral DNA clone MD14YE (ref. 21), with the HIV–1DH12 env gene. c, 32P RT assays showing neutralization of 100 TCID50 of SHIVDH12 in quadruplicate cultures as described11, with threefold serial dilutions of IgGs purified from chimpanzees chronically infected with HIV–1DH12 (Ch 1206) or HIV–1IIIB (Ch 911).
To formally demonstrate that chimpanzee IgG capable of neutralizing HIV–1DH12 could also neutralize a SHIV (SHIVDH12) bearing the HIV–1DH12 gp120, we did a neutralization assay using IgG purified from heparinized plasma of Ch 1206 (infected with HIV–1DH12) and Ch 911 (infected with HIV–1IIIB)(Fig. 1c). Serial threefold dilutions of the IgG preparations were incubated with 100 TCID50 (50% tissue culture infectious dose) of SHIVDH12 for 1 hour at room temperature, and the mixture was then used as the inocula for quadruplicate, 2–week infections of MT–4 cells. Non–neutralized culture supernatants appear as black dots on the autoradiograms of these 32P reverse transcriptase (RT) assays, reflecting the presence of (progeny) virus–associated RT activity in the medium. The absence of black dots indicates complete neutralization of virus infectivity, not merely the reduction of virus production. In the assay shown, SHIVDH12 infectivity was blocked at the higher concentrations of IgG from Ch 1206. The calculated23 neutralization titer (the dilution at which two of the quadruplicate infections would show neutralization, indicated by the absence of RT activity after 2 weeks of infection) of Ch 1206 IgG against 100 TCID50 of SHIVDH12 was 1:486 (Fig 1c). The neutralization titer of IgG from Ch 4750, the chimpanzee initially infected with three different HIV–1 isolates including HIV–1DH12, was in a similar range (data not shown). In contrast, IgG from Ch 911 had no detectable neutralizing activity against 100 TCID50 (Fig. 1c, right) or 10 TCID50 (data not shown) of SHIVDH12, although it was able to neutralize HIV–1IIIB (data not shown). All of the neutralization assays used (for convenience) MT4 cells, although, as reported24, high titers of neutralizing antibody directed against HIV–1DH12 are readily measured in chimpanzee serum using human PBMC.
The observed neutralization of SHIVDH12 by chimpanzee IgG is most likely mediated by antibodies targeting the HIV–1 envelope glycoproteins. Sera from SHIVDH12 infected rhesus monkeys, but not SIVΔ2– or SIVΔ3–infected macaques, readily neutralized SHIVDH12 (Ref. 11), indicating that Env– and not Gag–directed antibodies (both SIV and SHIV encode identical Gag proteins) were capable of blocking virus infectivity. Moreover, the IgG from chimpanzees 1206 and 4750, both previously infected with HIV–1DH12, and not the IgG purified from chimpanzee 911, chronically infected with HIV–1IIIB, neutralized the SHIV with the HIV–1DH12 envelope glycoprotein. This result is consistent with reports linking envelope sequence variability with differential susceptibilities to neutralizing antibodies25. Finally, serum from Ch 1206, which failed to neutralize the macrophage–tropic HIV–1Ada isolate, was able to neutralize chimeric HIV–1AD8/DH12, with gp160– (Ref. 24) or gp120–coding sequences from HIV–1 DH12, but not a chimeric virus expressing only the HIV–1DH12 gp41 (M.W.C., unpublished observations).
Monkeys immunized with whole inactivated SIV prepared in human lymphocytes or T–cell lines resist a subsequent virus challenge when the SIV inoculum is derived from human but not macaque cells26. In those studies, the target molecules for neutralization were most likely human lymphocyte–derived cell surface antigens incorporated into progeny virions during the budding process26. Here, the SHIVDH12 challenge stock was prepared in macaque PBMC, and none of the IgG donor chimpanzees had been previously exposed to macaque cells or proteins. Thus, the neutralizing activities associated with preparations of chimpanzee IgG target the HIV–1DH12 gp120 envelope glycoprotein. The neutralization assays here measure the 100% 'end points' of neutralization against a known titer of infectious virus. Unlike neutralization assays that measure 50% or 90% inhibition titers of virus–induced cytopathicity or the reduction of progeny virus produced from infected cells, the neutralization titers reported here represent the dilution of plasma that completely neutralizes the infectivity of input virus.
We initially studied the binding properties of the three chimpanzee IgG preparations to individual SHIVDH12 proteins by immunoblotting (Fig. 2). As expected, IgG from Ch 4750, originally infected with three HIV–1 isolates including HIV–1DH12, bound strongly to the gp120 and gp41 envelope proteins of SHIVDH12; cross–reactivity with the p27 Gag CA protein of SHIVDH12, derived from SIVmac239, was also seen. IgG from Ch 1206, despite having high titer neutralizing activity against SHIVDH12, showed only weak binding to the immobilized SHIVDH12 proteins at the two dilutions tested (Figs. 1c and 2). Weak binding of Ch 1206 IgG to SHIVDH12 proteins was also detected by ELISA (data not shown). Finally, IgG from Ch 911 (infected with HIV–1IIIB) showed binding activities to p27 CA similar to those of Ch 4750 IgG but less reactivity with the envelope proteins of SHIVDH12. The properties of the chimpanzee IgG used for passive transfer into pig–tailed macaques are summarized in Table 1.
The SHIVDH12 proteins in infected MT–4 cell lysates were resolved by SDS–PAGE and incubated with the indicated serially diluted chimpanzee IgG samples or the serum from a SHIVDH12 infected macaque (positive control). Right margin, the positions of the HIV–1 gp120 and gp41 envelope glycoproteins and the SIV p55, p28 and p17 Gag proteins.
In the initial in vivo challenge experiment, 100 TCID50 of SHIVDH12 was selected as the amount of virus to be intravenously inoculated after passive transfer of chimpanzee IgG. Based on a challenge dose of this size, we determined the amounts of IgG administered to macaque monkeys. The plasma volume of a 4–kg pig–tailed macaque is approximately 5% of its body weight, or 200 ml; therefore, the intravenous transfer of 0.5 ml of chimpanzee IgG would result in a 1:400 dilution during its distribution throughout the plasma. Based on the results of in vitro virus neutralization assays (Fig. 1c), the neutralizing activity present in 0.5 ml of Ch 1206 IgG or Ch 4750 IgG would be sufficient to neutralize 100 TCID50 of SHIVDH12 in plasma after passive transfer. However, because of uncertainties about further dilution of the administered IgG due to extravascular diffusion into other body compartments, we decided to administer tenfold more (5 ml) of Ch 1206 IgG and Ch 4750 IgG. The dose (17 ml) of IgG from the HIV–1IIIB–infected chimpanzee (Ch 911), which demonstrated no detectable neutralizing activity against SHIVDH12, was determined by normalizing its binding activity to SHIV proteins, deduced from quantitative ELISA and immunoblotting assays, to that of Ch 4750 IgG (Fig. 2 and Table 1). Finally, the total amount (306 mg) of IgG administered to each macaque was made equal by supplementation with IgG prepared from an uninfected chimpanzee (Ch 73). The half–life of chimpanzee IgG in pig–tailed macaques, determined by measuring the decay of anti–HIV gag antibody, was 10 to 14 days (data not shown).
In experiment 1, chimpanzee IgG was passively transferred to four pairs of pig–tailed macaques (Table 2). Blood was collected from the eight monkeys 24 hours after intravenous IgG administration (and immediately before the SHIVDH12 challenge), and plasma neutralization titers against 100 TCID50 of virus were determined ex vivo. Plasma from the four macaque recipients of IgG from chimpanzees chronically infected with HIV–1DH12 was able to neutralize SHIVDH12, with neutralizing titers ranging from 1:2.5 to 1:4 (Fig. 3a, top). In contrast, plasma from the two macaque recipients of IgG from Ch 73 (naive) and from the two monkeys given IgG from Ch 911 (HIV–1IIIB) failed to neutralize 100 TCID50 of SHIVDH12. As expected, the binding antibody titers in the plasma of the four macaques receiving Ch 4750 IgG or Ch 911 IgG, as measured by ELISA, were similar (approximately 1:2,000; Fig.3a, middle, and Table 2), whereas ELISA binding activity was undetectable in monkeys passively immunized with Ch 1206 IgG or Ch 73 IgG.
a (experiment 1), Serially diluted plasma samples were tested for neutralizing activity (top) against 100 TCID50 of SHIVDH12 and binding activity (middle), using an HIV–1 ELISA plate. Bottom, Donor chimpanzee ID numbers and IgG specificities. b (experiment 2), the neutralizing activities in serially diluted plasma samples from animals 94P010 and 94P011, challenged with 10 and 100 TCID50 of SHIVDH12, respectively.
The eight macaques were challenged intravenously with 100 TCID50 of SHIVDH12, and virus infectivity in vivo was monitored by quantitative DNA PCR of proviral DNA in PBMC. High–titer SHIV infections were established within 10 days of inoculation in recipients of either the naive or HIV–1IIIB IgG preparations (Fig. 4a). In contrast, virus infection was considerably delayed during this early period in the four animals passively immunized with the neutralizing IgG preparations. The proviral DNA loads in these macaques also tended to be lower at later times compared with the levels measured in the recipients of the naive or IIIB IgG (Fig. 4b). Animal 94P027 became only transiently infected (that is, was positive on days 14 and 28 and remains virus negative at week 54) after challenge with SHIVDH12 (Fig. 4b). These results indicate that passively transferred neutralizing IgG had some inhibitory effect on SHIVDH12 infections in vivo and that the quantities of Ch 1206 IgG and Ch 4750 IgG administered might have been 'borderline' for complete protection from infection.
a and b (experiment 1), PBMC–associated proviral DNA levels at day 10 (a) and over a 4–month period (b) after virus challenge. c (experiment 2), Viral DNA loads measured in two animals that received tenfold more IgG relative to that used in experiment 1 Quantitative DNA PCR was done as described17.
IgG from Ch 911 (HIV–1IIIB) conferred no resistance against the initial SHIVDH12 infection (compared with Ch 4750 IgG or Ch1206 IgG; Fig. 4a) nor did it enhance the subsequent SHIV infection (compared with the Ch 73 control IgG administered to macaques 94P018 and 94P025; Fig. 4b).
To determine whether the amount of the neutralizing IgG administered to the four monkeys was in fact 'borderline', we did a second passive transfer experiment involving two additional pig–tailed macaques (Table 2). One animal (94P011) was given tenfold more Ch 1206 IgG (50 ml) than that used previously and was challenged with 100 TCID50 of SHIVDH12. The second monkey (94P010) received the same amount (5 ml) of the Ch 1206 IgG administered in experiment 1, but was inoculated with tenfold less (10 TCID50) SHIVDH12. Chronic infections have been established infections in two of two pig–tailed macaques parenterally inoculated with 0.8 TCID50 of the SHIVDH12 stock (intravenously21 or after submucosal injection, R.O., unpublished data).
Ex vivo assays of samples collected 24 hours after IgG transfer had neutralization titers of 1:8 and 1:5 against 100 and 10 TCID50 of SHIVDH12, respectively, in the plasma of the two passively immunized monkeys studied in experiment 2 (Fig. 3b and Table 2). Complete protection from infection was achieved after subsequent SHIVDH12 challenge in both of these macaques (Fig. 4c): no PBMC–associated proviral DNA was detected in ten specimens analyzed over a 1–year period (the first 4 months after challenge are shown in Fig. 4c) and lymph nodes, biopsied in weeks 1 and 3, were negative by DNA PCR. Infectious virus could not be isolated from either PBMC or lymph node samples.
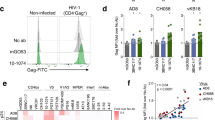
To reconcile the apparent discrepant neutralizing and immunoblotting properties of the Ch 1206 and Ch 911 IgGs (Table 1), we measured the direct binding of antibodies to 35S–methionine–labeled particles bearing the HIV–1DH12 envelope glycoprotein24,27,28. Radiolabeled virions were incubated under non–denaturing conditions with the non–neutralizing Ch 73 IgG and Ch 911 IgG or with the neutralizing Ch 4750 IgG and Ch 1206 IgG. The virion–IgG complex was then separated from any remaining free IgG and non–virion associated proteins by centrifugation24,27. The virion pellet was treated with 0.1% Triton X–100 and the HIV–1 proteins bound to chimpanzee IgGs were immunoprecipitated using protein A–agarose. The remaining supernatant, containing virion–associated proteins that had not bound to chimpanzee IgGs, were subsequently immunoprecipitated using AIDS patients' sera and protein A–agarose. The neutralizing IgGs (from Ch 4750 and Ch 1206) reacted with virion associated gp120 (Fig. 5a, left lanes), whereas the non–neutralizing IgGs from the naive and HIV–1IIIB infected chimpanzees did not (Fig. 5b, left lanes). The protein gp120 is in fact present in the non–binding fractions of HIV–1 proteins incubated with the non–neutralizing IgGs (Fig. 5b, right lanes). These results indicate that anti HIV–1 specific neutralizing antibodies are able to recognize and bind to native gp120 present on virus particles.
Radiolabeled HIV–1 virions were incubated with chimpanzee IgG and virion–associated proteins reactive with the various IgGs were immunoprecipitated. IgGs from HIV–1DH12 chimpanzee #1 (Ch 1206), HIV–1DH12 chimpanzee 2 (Ch 4750), HIV–1IIIB chimpanzee (Ch 911) and a naive chimpanzee (Ch 73). Left margin, the positions of the HIV–1 gp120 Env, p66 RT, p55 and p24 Gag, and p32 IN proteins.
An effective prophylactic vaccine for HIV–1 may have to elicit multiple immune responses (for example, CTLs, cytokine production, neutralizing antibodies) capable of interfering with different steps of the virus life cycle in vivo. Here we provide proof of the principle that anti–HIV–1 antibodies, capable of blocking virus infections in vitro, are by themselves protective in vivo. To achieve in vivo protection from infection by antibodies alone, the plasma of passively immunized animals had to be capable of completely neutralizing the intravenous challenge dose (measured in these experiment at a dilution of 1:5 to 1:8).Our end–point neutralization assay imposes a much more stringent readout than many assays commonly used, in which 90% reduction of p24 production on day 7 of infection is used to define the neutralization titer. Our results are consistent with a passive immunization study in which the protective titer in the hu–PBL–SCID mouse model corresponded to the 99% not the 90% p24 reduction titer measured in vitro22.
A chief shortcoming of our study is that we assessed only homologous combinations of challenge virus (SHIVDH12) and passively transferred IgGs (prepared from HIV–1DH12 infected chimpanzees). In addition, the molecularly cloned, dual–tropic HIV–1DH12 envelope target of the neutralization antibodies analyzed here may not be representative of a strict CCR5 chemokine coreceptor using gp120 associated with viral strains that initiate most acute infections in humans. We have identified a few sera from HIV–1 infected individuals and some broadly anti–HIV–1 neutralizing monoclonal antibodies that can neutralize HIV–1DH12 in vitro. A passive immunization study using 'heterologous' (cross–neutralizing) combinations might be useful. The passive transfer of a broadly neutralizing monoclonal antibody considerably delayed the establishment of an HIV–1 infection and reduced virus loads in two chimpanzees inoculated with a primary HIV–1 isolate30.
Passive immunization studies using animal challenge models have provided evidence that sufficient pre–existing titers of neutralizing antibody can completely block infection initiated by primary HIV–1 isolates (or SHIVs with a primary HIV–1 envelope). Although the experiments reported here must be replicated in a larger number of macaques using a variety of neutralizing IgG combinations and challenge virus strains, our results indicate that a vaccine capable of inducing sufficient levels of neutralizing antibody against HIV–1 clinical isolates could prevent the establishment of a virus infection.
Despite the promising results obtained and their implications for HIV–1 vaccine development, several essential questions remain. Can neutralizing antibodies confer resistance against a cell–associated virus challenge and/or mucosal challenge, and what neutralization titer is sufficient for protection? What is the size of a 'physiological' HIV–1 challenge dose, transmitted from an infected person to a naive recipient, that must be blocked by an effective prophylactic vaccine? It is certainly much less than 10–100 AID50, the dose commonly used in animal model studies like the one described here. Thus, the measurement of end–point neutralizing titers of human vaccinees against such a 'physiological' challenge dose may not be technically feasible. And finally, how does one formulate a vaccine that can induce sufficient neutralizing titers against a broad range of HIV–1 clinical isolates?
Methods
Animal experiments.
Pig–tailed macaques (Macaca nemestrina) and chimpanzees (Pan troglodytes) were maintained in accordance with the Guide for the Care and Use of Laboratory Animals31 and were housed in a biosafety level 2 facility; biosafety level 3 practices were followed. Animals were anesthetized with intramuscular injections of Tiletmine–HCl and Zolazepam–HCl (Telazol; Fort Dodge Laboratories, Fort Dodge, Iowa) during passive immunization, phlebotomy or virus inoculation.
Immunoglobulin fractions were purified from HIV–1 infected chimpanzees as described20. IgGs were administered intravenously 24 h before virus challenge. A portion (1 ml) of the appropriately diluted SHIVDH12 challenge stock was inoculated intravenously.
Virus load measurements were determined by quantitative DNA PCR analyses of PBMC and lymph node specimens from infected animals as described11.
The challenge virus.
An SHIV (ref. 21) derived from HIV–1DH12 was used for animal challenge experiments. HIV–1DH12 is a clade B, primary isolate capable of infecting and inducing syncytia in human T–cell lines and primary human macrophages17 and uses either CCR5 or CXCR4 as the co–receptor for infection28. Its derivative SHIVDH12 molecular clone, MD14YE (ref. 21), contains the LTR, gag, pol, vif, vpx and nef genes, and the first 17 codons of the vpr gene of SIVmac239. The tat, rev and env genes and the remainder of the vpr gene were derived mostly from HIV–1DH12, except for a small segment (145 bp) at the SIV/HIV–1 junction in vpr) that is of HIV–1NL4–3 origin. The SHIVDH12 MD14YE animal challenge stock (3 × 105 TCID50/ml; 86 ng p27 per ml), prepared in cultured macaque monkey PBMC, was diluted in RPMI medium to 100 TCID50/ml (or 10TCID50/ml), and 1 ml was used for intraveneous inoculation of macaques. The in vivo titration of this SHIVDH12 MD14YE stock in pig–tailed macaques has been reported21.
Antibody assays.
Neutralizing activities in the plasma of passively immunized monkeys were titered in an assay that measures 100% neutralization against known amounts of virus11. Here, the same amounts of SHIVDH12 were used for in vivo challenge (100 TCID50 or 10 TCID50) and for in vitro neutralization assays. The SHIVDH12 MD14YE animal challenge stock was initially diluted to 20,000 TCID50/ml (or to 2,000 TCID50/ml for neutralization assays in which 10 TCID50 of virus was used). Plasma samples were serially diluted (twofold or threefold, starting at a dilution of 1:2 or 1:6) in a mixture of pre–passive immunization plasma from the pig–tailed macaques. A 20–μl aliquot of each plasma dilution was incubated with 20 μl of SHIVDH12 at room temperature for 1 h and was then used to infect MT–4 cells in quadruplicate; each culture (5 × 104 MT–4 cells in 0.25 ml volume) received 10 μl of the virus/plasma mixture, which contained 100 (or 10) TCID50 of SHIVDH12. Infected cultures were maintained for 2 weeks and virus replication was monitored by 32P–reverse transcriptase assay29. After the 2–week incubation in MT–4 cells, any infectious SHIVDH12 would be amplified to levels detectable by the assay. In the experiment shown in Fig. 3b (left panel), three of four cultures at the 1:4 plasma dilution failed to produce detectable reverse transcriptase activitiy (complete neutralization). The plasma dilution at which two of the four cultures would be RT–negative (neutralization positive) was calculated to be 1:5, using the method of Reed and Munch23.
Binding antibodies to denatured HIV proteins were detected by a commercial ELISA kit (Vironostika HIV–1 Microelisa system; Organon Teknika, Durham, North Carolina). Immunoblots were analyzed using a Fuji phosphoimager (Fuji Medical System, Stamford, Connecticut) after incubation with 125I–labeled protein A (ICN) as described11.
To measure antibodies binding to native HIV–1DH12 virions, 35S–methionine–labeled particles, released from transfected HeLa cells24,27,28, were pelleted in an ultracentrifuge to remove non–particle associated viral proteins, resuspended in 100 μl of RPMI medium as described27,29 and incubated with 20 μg of the chimpanzee IgGs for 2 h at 37 °C. The HIV–1/IgG mixture was centrifuged27, the pellets were treated with 0.1% Triton X–100, and protein A–agarose was added to immunoprecipitate virion–associated proteins associated with the chimpanzee IgG. Supernatants from this immunoprecipitation were transferred to tubes containing protein A–agarose that had been pretreated with AIDS patients' sera for a second round of immunoprecipitation to assess the virion–associated proteins that did not bind to the chimpanzee IgG. The immunoprecipitated proteins were resolved by SDS–PAGE (ref. 27).
For immunoblotting of SHIV proteins using three different chimpanzee IgGs, the SHIVDH12 proteins present in infected MT–4 cell lysates were resolved by SDS–PAGE, transferred to nitrocellulose membranes, incubated with the indicated serially diluted chimpanzee IgG samples or the serum from a SHIVDH12 infected macaque (positive control) and visualized with a Fuji phosphoimager after incubation with 125I–protein A (ICN).
References
Hammon, W.M., Coriell, L.L., Wehrle, P.F. & Stokes Jr., J. Evaluation of Red Cross gamma globulin as a prophylactic agent of poliomyelitis: final report of results based on clinical diagnoses. J. Am. Med. Assoc. 151, 1272–1285 (1953).
Janeway, C.A. Use of concentrated human serum α–globulin in the prevention and attenuation of measles. Bull. NY Acad. Med. 21, 202–222 (1945).
Groothuis, J.R. et al. Prophylactic administration of respiratory syncytial virus immune globulin to high–risk infants and young children. The Respiratory Syncytial Virus Immune Globulin Study Group. N. Engl. J. Med. 329, 1524–1530 (1993).
Beasley, R. P. et al. Efficacy of hepatitis B immune globulin for prevention of perinatal transmission of the hepatitis B virus carrier state: final report of a randomized double–blind, placebo–controlled trial. Hepatology 3, 135–141 (1983).
Snydman, D. R. et al. Use of cytomegalovirus immune globulin to prevent cytomegalovirus disease in renal–transplant recipients. N. Engl. J. Med. 317, 1049–1054 (1987).
Krugman, S., Ward, R., Giles, J.P. & Jacobs, A.M. Infectious hepatitis: studies on the effect of gamma globulin and on the incidence of inapparent infection. J. Am. Med. Assoc. 174, 83– 90 (1960).
Virgin IV, H.W., Bassel–Duby, R., Fields, B.N. & Tyler, K.L. Antibody protects against lethal infection with the neurally spreading reovirus type 3 (Dearing). J. Virol. 62, 4594– 4604 (1988).
Johnson, R.P. Macaque models for AIDS vaccine development. Curr. Opin. Immunol. 8, 554–560 (1996).
Bogers, W.M. et al. Protection from HIV–1 envelope–bearing chimeric simian immunodeficiency virus (SHIV) in rhesus macaques infected with attenuated SIV: consequences of challenge. AIDS 9, F13–F18 (1995).
Shibata, R. et al. Resistance of previously infected chimpanzees to successive challenges with a heterologous intraclade B strain of human immunodeficiency virus type 1. J. Virol. 70, 4361– 4369 (1996).
Shibata, R., Siemon, C., Czajak, S.C., Desrosiers, R.C. & Martin, M.A. Live, attenuated simian immunodeficiency virus vaccines elicit potent resistance against a challenge with a human immunodeficiency virus type 1 chimeric virus. J. Virol. 71, 8141–8148 (1997).
Berman, P. W. et al. Protection of chimpanzees from infection by HIV–1 after vaccination with recombinant glycoprotein gp120 but not gp160. Nature 345, 622–625 (1990).
Bruck, C. et al. HIV–1 envelope–elicited neutralizing antibody titres correlate with protection and virus load in chimpanzees. Vaccine 12, 1141–1148 (1994).
Emini, E. A. et al. Prevention of HIV–1 infection in chimpanzees by gp120 V3 domain–specific monoclonal antibody. Nature 355, 728–730 (1992).
Girard, M. et al. Immunization of chimpanzees confers protection against challenge with human immunodeficiency virus. Proc. Natl. Acad. Sci. USA 88, 542–546 (1991).
Prince, A.M. et al. Prevention of HIV infection by passive immunization with HIV immunoglobulin. AIDS. Res. Hum. Retroviruses 7, 237–239 (1991).
Shibata, R. et al. Isolation and characterization of a syncytium–inducing, macrophage/T–cell line–tropic human immunodeficiency virus type 1 isolate that readily infects chimpanzee cells in vitro and in vivo. J. Virol. 69, 4453– 4462 (1995).
Shibata, R. et al. Reactivation of HIV type 1 in chronically infected chimpanzees following xenostimulation with human cells or with pulses of corticosteroid. AIDS Res. Hum. Retroviruses 13, 377– 381 (1997).
Arthur, L.O. et al. Challenge of chimpanzees (Pan troglodytes) immunized with human immunodeficiency virus envelope glycoprotein gp120. J. Virol. 63, 5046–5053 (1989).
Haigwood N.L. et al. Passive immune globulin therapy in the SIV/macaque model: early intervention can alter disease profile. Immunol. Lett. 51, 107–114 (1996).
Shibata, R. et al. Infection and pathogenicity of chimeric simian–human immunodeficiency viruses in macaques: determinants of high virus loads and CD4 cell killing. J. Infect. Dis. 176, 362–373 (1997).
Gauduin, M.C. et al. Passive immunization with a human monoclonal antibody protects hu–PBL–SCID mice against challenge by primary isolates of HIV–1. Nature Med. 3, 1389–1393 (1997).
Reed, L.J. & Muench, H. A simple method of estimating fifty percent endpoints. Am. J. Hyg. 27, 493– 497 (1938).
Willey, R.L., Shibata, R., Freed, E.O., Cho, M.W. & Martin, M.A. Differential glycosylation, virion incorporation, and sensitivity to neutralizing antibodies of human immunodeficiency virus type 1 envelope produced from infected primary T–lymphocyte and macrophage cultures. J. Virol. 70, 6431– 6436 (1996).
Moore, J. & Trkola, A. HIV type 1 coreceptors, neutralization serotypes, and vaccine development. AIDS Res. Hum. Retroviruses 13, 733–736 (1997).
Stott, E.J. Towards a vaccine against AIDS: lessons from simian immunodeficiency virus vaccines. Curr. Top. Microbiol. Immunol. 188, 221–237 (1994).
Willey, R.L., Martin, M.A. & Peden, K.W.C. Increase in soluble CD4 binding to and CD4–induced dissociation of gp120 from virions correlates with infectivity of human immunodeficiency virus type 1. J. Virol. 68, 1029– 1039 (1994).
Cho, M.W., Lee, M.K., Carney, M.C., Berson, J.F., Doms, R.W. & Martin, M.A. Identification of determinants on a dualtropic human immunodeficiency virus type 1 envelope glycoprotein that confer usage of CXCR4. J. Virol. 72, 2509–2515 (1998).
Willey, R.L., Klimkait, T., Frucht, D.M., Bonifacino, J.S. & Martin, M.A. Mutations within the human immunodeficiency virus type 1 gp160 envelope glycoprotein alter its itracellular transport and processing. Virology 184, 319– 329 (1991).
Conley, A.J. et al. The consequence of passive administration of an anti–human immunodeficiency virus type 1 neutralizing monoclonal antibody before challenge of chimpanzees with a primary virus isolate. J. Virol. 70, 6751–6758 (1996).
National Institutes of Health in Guide for the Care and Use of Laboratory Animals, revised ed. DHHS publication number NIH 85–23 (1985).
Acknowledgements
We thank A. Azadegan, W. Satterfield, A. Javadian and G. Coleman for assistance in the animal study; C. Pierce for the purification of immunoglobulin; T. Matthews, A. Trkola and J. Moore for providing information on neutralization assays; and R. Channock, B. Murphy and H. Ginsberg for discussions about virus neutralization.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Shibata, R., Igarashi, T., Haigwood, N. et al. Neutralizing antibody directed against the HIV–1 envelope glycoprotein can completely block HIV–1/SIV chimeric virus infections of macaque monkeys. Nat Med 5, 204–210 (1999). https://doi.org/10.1038/5568
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1038/5568
This article is cited by
-
Nonhuman primate models of human viral infections
Nature Reviews Immunology (2018)
-
A CD4-mimetic compound enhances vaccine efficacy against stringent immunodeficiency virus challenge
Nature Communications (2018)
-
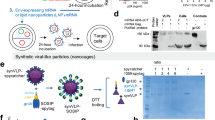
Enhancing Humoral Responses Against HIV Envelope Trimers via Nanoparticle Delivery with Stabilized Synthetic Liposomes
Scientific Reports (2018)
-
Functional effector memory T cells contribute to protection from superinfection with heterologous simian immunodeficiency virus or simian-human immunodeficiency virus isolates in Chinese rhesus macaques
Archives of Virology (2017)
-
A systems approach to HIV-1 vaccines
Nature Biotechnology (2016)