Summary
This paper presents the current state of knowledge on chloroquine disposition, with special emphasis on stereoselectivity and microsomal metabolism. In addition, the impact of the patient’s physiopathological status and ethnic origin on chloroquine pharmacokinetics is discussed.
In humans, chloroquine concentrations decline multiexponentially. The drug is extensively distributed, with a volume of distribution of 200 to 800 L/kg when calculated from plasma concentrations and 200 L/kg when estimated from whole blood data (concentrations being 5 to 10 times higher).
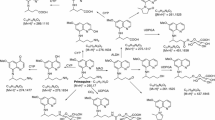
Chloroquine is 60% bound to plasma proteins and equally cleared by the kidney and liver. Following administration chloroquine is rapidly dealkylated via cytochrome P450 enzymes (CYP) into the pharmacologically active desethylchloroquine and bisdesethylchloroquine. Desethylchloroquine and bisdesethylchloroquine concentrations reach 40 and 10% of chloroquine concentrations, respectively; both chloroquine and desethylchloroquine concentrations decline slowly, with elimination half-lives of 20 to 60 days. Both parent drug and metabolite can be detected in urine months after a single dose.
In vitro and in vivo, chloroquine and desethylchloroquine competitively inhibit CYP2D1/6-mediated reactions. Limited in vitro studies and preliminary data from clinical experiments and observations point to CYP3A and CYP2D6 as the 2 major isoforms affected by or involved in chloroquine metabolism.
In vitro efficacy studies did not detect any difference in potency between chloroquine enantiomers but, in vivo in rats, S(+)-chloroquine had a lower dose that elicited 50% of the maximal effect (ED950) than that of R(−)-chloroquine. Stereoselectivity in chloroquine body disposition could be responsible for this discrepancy. Chloroquine binding to plasma proteins is stereoselective, favouring S(+)-chloroquine (67% vs 35% for the R-enantiomer). Hence, unbound plasma concentrations are higher for R(−)-chloroquine. Following separate administration of the individual enantiomers, R(−)-chloroquine reached higher and more sustained blood concentrations. The shorter half-life of S(+)-chloroquine appears secondary to its faster clearance. Blood concentrations of the S(+)-forms of desethylchloroquine always exceeded those of the R(−)-forms, pointing to a preferential metabolism of S(+)-chloroquine.
Similar content being viewed by others
References
White NJ, Nosten F. Advances in chemotherapy and prophylaxis of malaria. Curr Opin Infect Dis 1993; 6: 323–30
White NJ, Miller KD, Churchill FC, et al. Chloroquine treatment of severe malaria in children. Pharmacokinetics, toxicity, and new dosage recommendations. N Engl J Med 1988; 319: 1493–500
Bioland PB, Lackritz EM, Kazembe PN, et al. Beyond chloroquine: implications of drug resistance for evaluating malaria therapy efficacy and treatment policy in Africa. J Infect Dis 1993; 167: 932–7
Maksymovytch W, Russel AS. Antimalarials in rheumatology: efficacy and safety. Semin Arthritis Rheum 1987; 16: 206–21
Frisk-Holmberg M, Bergqvist Y, Domeij-Nyberg B, et al. Chloroquine serum concentration and side effects: evidence for dose-dependence kinetics. Clin Pharmacol Ther 1979; 25: 345–50
Frisk-Holmberg M, Bergqvist Y, Termond E. Further support for changes in chloroquine disposition and metabolism between a low and high dose. Eur J Clin Pharmacol 1985; 28: 721–2
Frisk-Holmberg M, Bergqvist Y. Chloroquine disposition in man. Br J Clin Pharmacol 1982; 14 Suppl.: 624–6
Frisk-Holmberg M, Bergqvist Y, Termond E, et al. The single dose kinetics of chloroquine and its major metabolite desethylchloroquine in healthy subjects. Eur J Clin Pharmacol 1984; 26: 521–30
Tett SE, Cutler DJ. Apparent dose-dependence of chloroquine pharmacokinetics due to limited assay sensitivity and limited sampling times. Eur J Clin Pharmacol 1987; 31: 729–31
Gustafsson LL, Rombo L, Alvan G, et al. On the question of dose-dependent chloroquine elimination of a single oral dose. Clin Pharmacol Ther 1983; 34: 383–5
Gustafsson LL, Bergqvist Y, Ericsson O, et al. Pitfalls in the measurement of chloroquine concentrations. Lancet 1983; I: 126
Adelusi SA, Salako LA. Improved fluorimetric assay of chloroquine in biological samples. J Pharm Pharmacol 1980; 32: 711–2
Alvan G, Ekman N, Lindstrom B. Determination of chloroquine and its desethyl metabolite in plasma, red blood cells and urine by liquid chromatography. J Chromatogr 1982; 229: 241–7
Geary TG, Akood MA, Jensen JB. Characteristics of chloroquine binding to glass and plastic. Am J Trop Med Hyg 1983; 32: 19–23
McChesney EW, Fasco MG, Banks WF. The metabolism of chloroquine in man during and after repeated oral dosage. J Pharmacol Exp Ther 1967; 158: 323–31
Bergqvist Y, Domeij-Nyberg B. Distribution of chloroquine and its major metabolite desethyl-chloroquine in human blood cells and its implication for the quantitative determination of these compounds in serum and plasma. J Chromatogr 1983; 272: 137–48
French JK, Hurst NP, O’Donnell ML, et al. Uptake of CQ and HCQ by human blood leucocytes in vitro: relation to cellular concentrations during antirheumatic therapy. Ann Rheum Dis 1987; 46: 42–5
McChesney EW, Conway WD, Banks WF, et al. Studies of the metabolism of some compounds of the 4-amino-7-chloroquine series. J Pharm Exp Ther 1966; 151: 482–93
Krishna S, White NJ. Pharmacokinetics of quinine, chloroquine and amodiaquine: clinical implications. Clin Pharmacokinet 1996; 30: 263–99
Gustafsson LL, Walker O, Alvan G, et al. Disposition of chloroquine in man after single intravenous and oral doses. Br J Clin Pharmacol 1983; 15: 471–9
De Vries PJ, Oosterhuis B, Van Boxtel CJ. Single-dose pharmacokinetics of chloroquine and its main metabolite in healthy volunteers. Drug Invest 1994; 8: 143–9
Wetsteyn JCFM, De Vries PJ, Oosterhuis B, et al. The pharmacokinetics of three multiple dose regimens of chloroquine: implications for malaria chemoprophylaxis. Br J Clin Pharmacol 1995; 39: 696–9
Rombo L, Ericsson O, Alvan G, et al. Chloroquine and desethylchloroquine in plasma, serum, and whole blood: problems in assay and handling of samples. Ther Drug Monit 1985; 7: 211–5
McChesney EW, Shekosky JM, Hernandez PH. Metabolism of chloroquine-3-14C in the rhesus monkey. Biochem Pharmacol 1967; 16: 2444–7
Grundmann M, Mikulikova I, Vrublovsky P. Tissue distribution of subcutaneously administered chloroquine in the rat. Arzneimittelforschung 1971; 21: 573–4
MacKenzie AH. Pharmacologic actions of 4-aminoquinoline compounds. Am J Med 1983; 75 Suppl. 1: 5–10
Robinson AE, Coffer AI, Camps FE. The distribution of chloroquine in man after fatal poisoning. J Pharm Pharmacol 1970; 22: 700–3
Larsson B, Tjalve H. Studies on the mechanism of drug-binding to melanin. Biochem Pharmacol 1979; 28: 1181–7
Thompson PE, Werbel LM. Antimalarial agents. New York: Academic Press, 1972: 150–96
Titus EO. Recent developments in the understanding of the pharmacokinetics and mechanism of action of chloroquine. Ther Drug Monit 1989; 11: 369–79
Yayon A, Cabantchick ZI, Ginsberg H. Identification of the acidic compartment of Plasmodium falciparum-infected erythrocytes as the target of the antimalarial drug chloroquine. EMBO J 1984; 3: 2695–700
Keen JH, Willingham MC, Pastan IH. Clathrin-coated vesicles: isolation, dissociation, and factor-dependent reassociation of clathrin baskets. Cell 1979; 16: 303–12
Ferrari V, Cutler DJ. Kinetics and thermodynamics of chloroquine and hydroxychloroquine transport across the human erythrocyte membrane. Biochem Pharmacol 1991; 40: 23–30
MacIntyre AC, Cutler DJ. The potential role of lysosomes in tissue distribution of weak bases. Biopharm Drug Dispos 1988; 9: 513–26
Veignie E, Moreau S. The mode of action of chloroquine. Non-weak base properties of 4-aminoquinolines and antimalarial effects on strains of Plasmodium. Ann Trop Med Parasitol 1991; 85: 229–37
Krogstad DJ, Schlessinger PH, Gluzman IY. Antimalarials increase vesicle pH in Plasmodium falciparum. J Cell Biol 1985; 101: 2302–9
Moreau S, Prensier G, Maalla J, et al. Identification of distinct accumulation sites of 4-aminoquinoline in chloroquine sensitive and resistant Plasmodium berghei strains. Eur J Cell Biol 1986; 42: 207–10
Augustjins P, Geusens P, Verbeke N. Chloroquine levels in blood during chronic treatment of patients with rheumatoid arthritis. Eur J Clin Pharmacol 1992; 42: 429–33
Ofori-Adjei D, Ericsson O, Lindstrom B, et al. Protein binding of chloroquine enantiomers and desethylchloroquine. Br J Clin Pharmacol 1986; 22: 356–8
Augustijns P, Verbeke N. Stereoselective pharmacokinetic properties of chloroquine and de-ethyl-chloroquine in humans. Clin Pharmacokinet 1993; 24: 259–69
Walker O, Birkett DJ, Alvan G, et al. Characterization of chloroquine plasma protein binding in man. Br J Clin Pharmacol 1983; 15: 375–7
Gustafsson LL, Lindstrom B, Grahnen A, et al. Chloroquine excretion following malaria prophylaxis. Br J Clin Pharmacol 1987; 24: 221–4
Ofori-Adjei D, Ericsson O. Chloroquine in nail clippings [letter]. Lancet 1985; II: 331
Frisk-Holmberg M, Bergqvist Y, Termond E. Further support for changes in chloroquine disposition between a low and a high dose. Eur J Clin Pharmacol 1985; 28: 721–2
Frisk-Holmberg M, Bergqvist Y, Domeij-Nyberg B. Steady-state disposition of chloroquine in patients with rheumatoid disease. Eur J Clin Pharmacol 1983; 24: 837–9
Frisk-Holmberg M, Bergqvist Y, Termond E, et al. The single dose kinetics of chloroquine and its major metabolite desethyl-chloroquine in healthy subjects. Eur J Clin Pharmacol 1984; 26: 521–30
Price-Evans DA, Fletcher KA, Baty ID. The urinary excretion of chloroquine in different ethnic groups. Ann Trop Med Parasitol 1979; 73: 11–7
Ette EI, Essien EE, Thomas WOA, et al. Pharmacokinetics of chloroquine and some of its metabolites in healthy volunteers: a single dose study. J Clin Pharmacol 1989; 29: 457–62
Bennett WM, Aronoff GR, Golper TA, et al. Drug prescribing in renal failure. Philadelphia: American College of Physicians, 1987
Hellgren U, Alvan G, Jerling M. On the question of interindividual variations in chloroquine concentrations. Eur J Clin Pharmacol 1995; 45: 383–5
Bergqvist Y, Frisk-Holmberg M. Sensitive method for the determination of chloroquine and its metabolite desethylchloroquine in human plasma and urine by high performance liquid chromatography. J Chromatogr 1980; 221: 119–27
Augustijns P, Verbeke N. HPLC method for the determination of chloroquine and its main metabolite in biological samples. J Liq Chromatogr Clin Analysis 1990; 13: 1203–13
Adelusi SA, Salako LA. Tissue and blood concentrations of chloroquine following chronic administration in the rat. J Pharm Pharmacol 1982; 34: 733–5
Lancaster DL, Adio RA, Tai KK, et al. Inhibition of metoprolol metabolism by chloroquine and other antimalarial drugs. J Pharm Pharmacol 1990; 42: 267–71
Masimirembwa CM, Hasler JA, Johansson I. Inhibitory effects of antiparasitic drugs on cytochrome P450 2D6. Eur J Clin Pharmacol 1995; 48: 35–8
Halliday RC, Jones BC, Smith DA, et al. An investigation of the interaction between halofantrine, CYP2D6 and CYP3A4: studies with human liver microsomes and heterologous enzyme expression systems. Br J Clin Pharmacol 1995; 40: 369–78
Koymans L, Vermeulen NPE, van Acker SABE, et al. A predictive model for substrates of cytochromes P450-debrisoquine (2D6). Chem Res Toxicol 1992; 5: 211–9
Mikus G, Ha AR, Vozeh S, et al. Pharmacokinetics and metabolism of quinidine in extensive and poor metabolisers of sparteine. Eur J Clin Pharmacol 1986; 31: 69–72
Evans DA, Mahgoub A, Sloan TP, et al. A family and population study of the genetic polymorphism of debrisoquin oxidation in a white British population. J Med Genet 1980; 17: 102–5
Eichelbaum M, Gross AS. The genetic polymorphism of debrisoquine/sparteine metabolism, clinical aspects. In: Kalow W, editor. Pharmacogenetics of drug metabolism. New York: Pergamon Press, 1992: 625–48
Bertilsson L. Geographical/interracial differences in polymorphic drug oxidation: current state of knowledge of cytochromes P450 (CYP) 2D6 and 2C19. Clin Pharmacokinet 1995; 29: 192–209
Daniel W, Netter KJ. Alteration of cytochrome P450 by prolonged administration of imipramine and/or lithium to rats. Naunyn Schmiedebergs Arch Exp Pathol Pharmacol 1990; 342: 234–40
Masubichi Y, Takahashii C, Fujio N, et al. Inhibition and induction of cytochrome P450 isozymes after repetitive administration of imipramine in rats. Drug Metab Dispos 1995; 23: 999–1003
Onyeji CO, Toriola TA, Ogunbona FA. Lack of pharmacokinetic interaction between chloroquine and imipramine. Ther Drug Monit 1993; 15: 43–6
Masimirembwa CM, Gustafsson LL, Dahl ML, et al. Lack of effect of chloroquine on the debrisoquine (CYP2D6) and S-mephenytoin (CYP2C19) hydroxylation phenotypes. Br J Clin Pharmacol 1996; 41: 344–6
Ette EI, Brown-Awala EA, Essien EE. Chloroquine elimination in humans: effect of low-dose cimetidine. J Clin Pharmacol 1987; 27: 813–6
Knodell RG, Holtzman JL, Crankshaw DL, et al. Drug metabolism by rat and human hepatic microsomes in response to interaction with H2-receptor antagonists. Gastroenterology 1982; 82: 84–8
Ortiz de Montellano PR, Reich NO. Inhibition of cytochrome P-450 enzymes. In: Ortiz de Montellano PR, editor. Cytochrome P-450: structure, mechanism and biochemistry. New York: Plenum, 1986: 273–314
Knodell RG, Browne DG, Gwozdz GP, et al. Differential inhibition of individual human liver cytochromes P-450 by cimetidine. Gastroenterology 1991; 101: 1680–91
Ette EI, Brown-Awala EA, Essien EE. Effect of ranitidine on chloroquine disposition. Drug Intell Clin Pharm 1987; 21: 732–4
Klotz U, Kroemer HK. The drug interaction potential of ranitidine: an update. Pharmacol Ther 1991; 50: 233–44
Nampoory MRN, Nessim J, Gupta RK, et al. Drug interaction of chloroquine with ciclosporin. Nephron 1992; 62: 108–9
Filniez P, Gendoo Z, Chuet C, et al. Interaction between cyclosporin and chloroquine. Nephron 1993; 65: 33
Combalbert J, Fabre I, Fabre G, et al. Metabolism of cyclosporin: IV-Purification and identification of the rifampicin-inducible human liver cytochrome P-450 (cyclosporin oxidase) as a product of P450IIIA gene subfamily. Drug Metab Biol Fate Chem 1989; 17: 197–207
Kolars JC, Schmiedlin-Ren P, Schuetz JD, et al. Identification of rifampicin-inducible P450IIIA4 (CYP3A4) in human small bowel enterocytes. J Clin Invest 1992; 90: 1871–8
Mwankwo JO, Garba MA, Chinje CE, et al. Possible chloroquine-induced modification of N-acetylation of isoniazid and sulphadimidine in the rat. Biochem Pharmacol 1990; 40: 654–9
Svensson CK, Zaher H, Tomilo M. Disposition of sulfamethazine and N-acetylsulfamethazine in the rat. Pharm Res 1991; 8: 1069–70
Lindsay RM, Baty JD. The effect of streptozotocin-induced diabetes on the in vivo acetylation capacity and the in vitro blood N-acetyltransferase activity of the adult male Sprague-Dawley rat. Biochem Pharmacol 1990; 39: 1193–7
Svensson CK, Drobitch RK, Tomilo M. Effects of chloroquine and primaquine on rat liver cytosolic N-acetyltransferase activity. Biochem Pharmacol 1991; 42: 954–6
Pacifici DM, Donatelli P, Giuliani L. Histamine N-methyltransferase: inhibition by drugs. Br J Clin Pharmacol 1992; 34: 322–7
Donatelli P, Marchi G, Giuliani L, et al. Stereoselective inhibition by chloroquine of histamine N-methyltransferase in the human liver and brain. Eur J Clin Pharmacol 1994; 47: 345–9
Adelusi SA, Dawodu AH, Salako L. Kinetics of the uptake and elimination of chloroquine in children with malaria. Br J Clin Pharmacol 1982; 14: 483–7
Walker O, Dawodu AH, Adeyokunnu AA, et al. Plasma chloroquine and desethylchloroquine concentrations in children during and after chloroquine treatment for malaria. Br J Pharmacol 1983; 16: 701–5
Na-Bangchang K, Limpaibul L, Tan-Ariya ATP, et al. The pharmacokinetics of chloroquine in healthy Thai subjects and patients with Plasmodium vivax malaria. Br J Clin Pharmacol 1994; 38: 278–81
Edwards G, Looareesuwan S, Davies A, et al. Pharmacokinetics of chloroquine in Thais: plasma and red cell concentrations following an intravenous infusion to healthy subjects and patients with Plasmodium vivax malaria. Br J Clin Pharmacol 1988; 25: 477–85
White NJ, Looareesuwan S, Warrell SA, et al. Quinine pharmacokinetics and toxicity in cerebral and uncomplicated falciparum malaria. Am J Med 1982; 73: 564–71
Warhurst DC. The quinine-haemin interaction and its relationship to antimalarial activity. Biochem Pharmacol 1981; 30: 3323–7
White NJ. Clinical pharmacokinetics of antimalarial drugs. Clin Pharmacokinet 1985; 10: 187–215
Silamut K, Molunto P, Ho M, et al. α1-Acid glucoprotein (orosomucoid) and plasma protein binding of quinine in falciparum malaria. Br J Clin Pharmacol 1991; 32: 311–5
White NJ, Watt G, Bergqvist Y, et al. Parenteral chloroquine for treating falciparum malaria. J Infect Dis 1987; 155: 192–201
Trenholme GM, Williams RL, Rieckmann KH, et al. Quinine disposition during malaria and during induced fever. Clin Pharmacol Ther 1976; 19: 459–67
Skirrow MR, Chongsuphajaisiddhi T, Maegraith BG. The circulation in malaria. II. Portal angiography in monkeys (Macaca mulatto) with P. knowlesi and in shock following manipulation of the gut. Ann Trop Med Parasitol 1964; 58: 502–10
Aikawa M, Susuki M, Gutierrez Y. Pathology of malaria. In: Kreier JP, editor. Malaria. Vol 2. New York: Academic Press, 1980: 47–102
Verdier F, Clavier F, Deloron P, et al. Distribution de la chloroquine et de la desethylchloroquine dans le sang, le plasma et les erythrocytes de sujets sains et paludeens. Pathol Biol 1984; 32: 359–61
Tulpule A, Krishnaswamy K. Chloroquine kinetics in the undernourished. Eur J Clin Pharmacol 1983; 24: 273–6
Walker O, Dawodu AH, Salako LA, et al. Single dose disposition of chloroquine in Kwashiorkor and normal children-evidence for decreased absorption in Kwashiorkor. Br J Clin Pharmacol 1987; 23: 467–2
Buchanan H, Van der Walt LA. The binding of chloroquine to normal and Kwashiorkor serum. Am J Trop Med Hyg 1977; 26: 1025–7
Koizumi A, Weindruch R, Walford RL. Influences of dietary restriction and age on liver enzyme activities and lipid peroxidation in mice. J Nutr 1987; 117: 361–5
Adelusi SA. Urinary levels of chloroquine in relation to dietary protein. Experientia 1982; 38: 1326–7
Mahmoud BM, Ali HM, Homeida MA, et al. Significant reduction in chloroquine bioavailability following coadministration with the Sudanese beverages Aradaib, Karkadi and Lemon. J Antimicrob Chemother 1994; 33: 1005–9
Tulpule A, Krishnaswamy K. Effect of food on bioavailability of chloroquine. Eur J Clin Pharmacol 1982; 23: 271–3
Fadeke-Aderounmu A, Salako LA, Lindstrom B, et al. Comparison of the pharmacokinetics of chloroquine after single intravenous and intramuscular administration in healthy Africans. Br J Clin Pharmacol 1986; 22: 559–64
Adjepon-Yamoah KK, Ofori-Adjei D, Woolhouse NM, et al. Whole blood single-dose kinetics of chloroquine and desethylchloroquine in Africans. Ther Drug Monit 1986; 8: 195–9
Bertilsson L, Lou YQ, Du YL, et al. Pronounced differences between native Chinese and Swedish populations in the polymorphic hydroxylations of debrisoquine and S-mephenytoin. Clin Pharmacol Ther 1992; 51: 388–97
Iyun AO, Lennard MS, Tucker GT, et al. Metoprolol and debrisoquine metabolism in Nigerians: lack of evidence for polymorphic oxidation. Clin Pharmacol Ther 1986; 40: 387–94
Mbanefo, C, Bababunmi EA, Mahgoub A, et al. a study of the debrisoquine hydroxylation polymorphism in a Nigerian population. Xenobiotica 1980; 10: 811–8
Akintonwa A, Gbajumo SA, Biola Mabadeje AF. Placental and milk transfer of chloroquine in humans. Ther Drug Monit 1988; 10: 147–9
Levy M, Buskila D, Gladman DD, et al. Pregnancy outcome following first trimester exposure to chloroquine. Am J Perinatol 1991; 8: 174–8
Wolfe MS, Cordero JF. Safety of chloroquine in chemosuppression of malaria during pregnancy. BMJ 1985; 290: 1466–7
Leng JJ, Mbanzulu PN, Akbaraly JP, et al. Etude in vitro du passage transplacentaire du sulfate de chloroquine. Pathol Biol 1987; 35: 1051–4
Akintonwa A, Meyer MC, Yau KT. Placental transfer of chloroquine in pregnant rabbits. Res Commun Chem Pathol Pharmacol 1983; 40: 443–55
O’Brien TE. Excretion of drugs in human milk. Am J Hosp Pharm 1974; 31: 844–54
Edstein MD, Veenendaal JR, Newman K, et al. Excretion of chloroquine, dapsone and pyrimethamine in human milk. Br J Clin Pharmacol 1986; 22: 733–5
Ogunbona FA, Onyeji CO, Bolaji OO, et al. Excretion of chloroquine and desethylchloroquine in human milk. Br J Clin Pharmacol 1987; 23: 473–6
Deturmeny E, Viala A, Durand A et al. Le passage de la chloroquine dans le lait, sur 1 cas. Therapie 1984; 39: 438–40
Fadeke-Aderounmu A. In vitro assessment of the antimalarial activity of chloroquine and its major metabolites. Ann Trop Med Parasitol 1984; 78: 581
Fu S, Bjorkman, Wahlin B, et al. In vitro activity of chloroquine, the two enantiomers of chloroquine, desethylchloroquine and pyronaridine against Plasmodium falciparum. Br J Clin Pharmacol 1986; 22: 93–6
Kyle DE, Oduola AMJ, Martin SK, et al. Plasmodium falciparum: modulation by calcium antagonists of resistance to chloroquine, desethylchloroquine, quinine and quinidine in vitro. Trans R Soc Trop Med Hyg 1990; 84: 474–8
Ladipo GOA, Essien EE, Andy JJ. Complete heart block in chronic chloroquine poisoning. Int J Cardiol 1983; 4: 198–200
Essien EE, Ette EI. Effects of chloroquine and desethylchloroquine on rabbit myocardium and mitochondria. J Pharm Pharmacol 1986; 38: 833–40
Peters W. The prevention of antimalarial drug resistance. Pharmacol Ther 1990; 47: 488–508
Martin SK, Oduola AMJ, Milhous WK. Reversal of chloroquine resistance in Plasmodium falciparum by verapamil. Science 1987; 235: 899–901
Yayon A, Cabantchik ZI, Ginsburg H. Susceptibility of human malaria parasites to chloroquine is pH dependent. Proc Natl Acad Sci USA 1985; 82: 2784–8
Krogstad DJ, Gluzman IY, Kyle DE, et al. Efflux of chloroquine from Plasmodium falciparum: mechanism of chloroquine resistance. Science 1987; 238: 1283–5
Pastan I, Gottesman M. Multiple-drug resistance in human cancer. N Engl J Med 1987; 316: 1388–93
Martiney JA, Cerami A, Slater AFG. Verapamil reversal of chloroquine resistance in the malaria parasite Plasmodium falciparum is specific for resistant parasites and independent of the weak base effect. J Biol Chem 1995; 270: 22393–8
Thiebaut F, Tsuruo T, Hamada H, et al. Cellular localization of the multidrug-resistance gene product P-glycoprotein in normal human tissues. Proc Natl Acad Sci USA 1987; 84: 7735–8
Murray GI, Barnes TS, Sewell HF, et al. The immunocytochemical localization and distribution of cytochrome P-450 in normal human hepatic and extrahepatic tissues with a monoclonal antibody to human cytochrome P-450. Br J Clin Pharmacol 1988; 25: 465–75
Cowan KH, Batist G, Tulpule A, et al. Similar biochemistry changes associated with multidrug resistance in human breast cancer cells and carcinogen-induced resistance to xenobiotics in rats. Proc Natl Acad Sci USA 1986; 83: 9328–32
Rushing DA, Raber SR, Rodvold KA, et al. The effects of cyclophosphamide on the pharmacokinetics of doxorubicin in patients with small cell lung cancer. Cancer 1994; 74: 834–41
Kronbach T, Fischer V, Meyer UA, et al. Cyclosporin metabolism in human liver: identification of a cytochrome P450III gene family as the major cyclosporin-metabolizing enzyme explains interactions of cyclosporin with other drugs. Clin Pharmacol Ther 1988; 43: 630–5
Mani C, Gelboin HV, Park SS, et al. Metabolism of the antimammary cancer antiestrogenic agent tamoxifen. I. Cytochrome P-450-catalyzed N-demethylation and 4-hydroxylation. Drug Metab Dispos 1993; 21: 645–56
Jacolot F, Simon I, Dreano Y, et al. Identification of the cytochrome P450 MA family as the enzymes involved in the N-demethylation of tamoxifen in human liver microsomes. Biochem Pharmacol 1991; 41: 1911–9
Scambia G, Ranelleti FO, Panici PB, et al. Quercetin potentiates the effect of adriamycin in a multidrug-resistant MCF-7 human breast cancer cell line; P-glycoprotein as a possible target. Cancer Chemother Pharmacol 1994; 34: 459–64
Rashid J, McKinstry C, Renwick AG, et al. Quercetin, an in vitro inhibitor of CYP3A, does not contribute to the interaction between nifedipine and grapefruit juice. Br J Clin Pharmacol 1993; 36: 460–3
Salganik RI, Pankova TG, Chekhonadskiku TW, et al. Chloroquine resistance of Plasmodium berghei: biochemical basis and counter measures. Bull World Health Organ 1987; 65: 381–6
Rabinovich SA, Kulikovskaya IM, Maksakovskaya EV, et al. Suppression of the chloroquine resistance of Plasmodium berghei by the treatment of infected mice with microsomal monooxygenase inhibitor. Bull World Health Organ 1987; 65: 387–9
Ndifor AM, Howells RE, Bray PG, et al. Enhancement of drug susceptibility in Plasmodium falciparum in vitro and Plasmodium berghei in vivo by mixed-function oxidase inhibitors. Antimicrob Agents Chemother 1993; 37: 1318–23
Von Fink E, Minet G, Nickel P. Chloroquine enantiomers, activity against P. vinckei and binding on DNA. Arzneimittel Forschung 1979; 29: 163–4
Haberkorn A, Kraft HP, Blaschke G. Antimalarial activity in animals of the optical isomers of chloroquine diphosphate. Tropenmed Parasitol 1979; 30: 308–12
McLachlan AJ, Cutler DJ, Tett SE. Plasma protein binding of the enantiomers of hydroxychloroquine and metabolites. Eur J Clin Pharmacol 1993; 44: 401–4
Brocks DR, Skeith KJ, Johnston C, et al. Hematologic disposition of hydroxychloroquine enantiomers. J Clin Pharmacol 1994: 34: 1088–97
Ofori-Adjei D, Ericsson O, Lindstrom B, et al. Enantioselective analysis of chloroquine and desethylchloroquine after oral administration of racemic chloroquine. Ther Drug Monit 1986; 8: 457–61
Ducharme J, Fieger H, Ducharme MP, et al. Enantioselective disposition of hydroxychloroquine after a single oral dose of the racemate to healthy subjects. Br J Clin Pharmacol 1995; 40: 127–33
McLachlan AJ, Tett SE, Cutler DJ, et al. Disposition of the enantiomers of hydroxychloroquine in subjects with rheumatoid arthritis following multiple doses of the racemate. Br J Clin Pharmacol 1993; 36: 78–81
Augustijns P, Verbeke N. Stereoselectivity in the disposition of chloroquine and desethylchloroquine in rabbits. Arzneimittel Forschung 1992; 42: 825–8
Augustijns P, Geusens P, Verbeke N. Chloroquine pharmacokinetic data during chronic daily treatment [reply to the letter by McLachlan et al.]. Eur J Clin Pharmacol 1993; 44: 409–10
Wainer I, Chen JC, Parenteau HI, et al. Distribution of the enantiomers of hydroxychloroquine and its metabolites in ocular tissues of the rabbit after oral administration of racemic hydroxychloroquine. Chirality 1994; 6: 347–54
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Ducharme, J., Farinotti, R. Clinical Pharmacokinetics and Metabolism of Chloroquine. Clin-Pharmacokinet 31, 257–274 (1996). https://doi.org/10.2165/00003088-199631040-00003
Published:
Issue Date:
DOI: https://doi.org/10.2165/00003088-199631040-00003